|
Greener Journal of Medical Sciences
Vol. 11(1), pp. 73-87, 2021
ISSN: 2276-7797
Copyright ©2021, the copyright of
this article is retained by the author(s)
https://gjournals.org/GJMS
|

|
The
Relationship between Fetal Umbilical Cord Length and Fetal Outcome
Maduagwu AO1; Okonkwo C2;
Onyegbule O1; Egwim
VA1; Ejelonu TU1
Department of Obstetrics and Gynaecology, Federal Medical Center, Owerri.1
Department of Obstetrics and Gynaecology, University of Benin Teaching Hospital.2
|
ARTICLE INFO
|
ABSTRACT
|
|
Article No.: 041621036
Type: Research
|
Background: The umbilical cord develops from the
extra-embryonic mesoderm and becomes the channel for blood vessels and
through which all exchange and other activities of mother and fetus through placenta are carried out. At term normal
umbilical cord length is about 50-70cm and with a diameter of 2.0-2.5cm.
There seems to be a positive correlation between fetal
umbilical cord length and fetal outcome.
Aim: The aim of the study was to determine the correlation between fetal umbilical cord length and the fetal
outcome at the Federal Medical Center, Owerri.
Methodology: This was a cross-sectional study of 427
parturient at term who will meet the eligibility criteria for the study. The
socio-demographic information were coded and
analysed using the Statistical Packages for Social Sciences (SPSS) version
23.
Results: The mean fetal umbilical cord length in this
study was 60.35cm + 10.39cm. the shortest fetal umbilical cord length was 33cm and the longest
umbilical cord length was 120cm.. There was poor correlation between birth
length and different umbilical cord length. There was a positive correlation
between birth length and normal fetal umbilical cord length(r=0.219) and between birth
length and long umbilical cord length(r=0.378).The correlation between birth
weight and different fetal umbilical cord length
showed a positive correlation between birth weight and normal umbilical cord
length(r=0.084) and long umbilical cord length(r=0.2467) There was poor
positive correlation between APGAR score and short umbilical cord length(r=0.333)
as well as between APGAR score and normal umbilical cord length(r=0.034). In
overall, the total abnormal fetal umbilical cord
length in this study was 4.9%. Also the overall prevalence of cord
complication in this study was 3.7%, and the prevalence of cord complication
was found to be higher in neonates with abnormal fetal
umbilical cord length (P<0.0001, χ2= 1.457). The fetal out come between abnormal fetal
umbilical cord length and normal umbilical cord length was statistically
significant (P<0.0001).
There was significant
association between different cord complication and fetal
umbilical cord length status (P<0.0006,
χ2= 18.288).
Conclusion; The study showed that the fetal umbilical cord length is variable. The maximum
number of cases had normal umbilical cord length. Abnormal umbilical cord
length had higher prevalence of cord complication. There are
significant positive correlation between fetal
umbilical cord length with birth weight, birth length.
|
|
Accepted: 16/04/2021
Published: 29/04/2021
|
|
*Corresponding Author
Dr.
Maduagwo AO
Email: anslemobitex@ gmail,com; nslemoitex@
gmail.com
|
|
Keywords: relationship;
fetal; umbilical; cord; length; outcome
|
|
|
|
INTRODUCTION
The umbilical cord1 is a conduit
between the developing embryo or fetus and the placenta. During the prenatal
development, the umbilical cord is physiologically and genetically part of the
fetus and normally contains two arteries (umbilical arteries) and one vein (the
umbilical vein) buried within the Whaton’s Jelly.
The umbilical cord
develops from the remnants of the yolk sac and allantois. It forms by the fifth
week of fetal development, replacing the yolk sac as the source of nutrients
for the fetus. The umbilical cord is not directly connected to the mother’s
circulatory system but instead joins the placenta, which transfers nutrients to
and from the mother’s blood without allowing direct mixing2.
The umbilical cord
and placenta has been considered to contribute significantly to perinatal
outcome3. However, in our environment, attempts at studying the
umbilical cord have been limited due to paucity of information on the
importance of the umbilical cord during the antenatal period and this issue is
further worsened by the prevailing socio-cultural believe which ensure that
umbilical cord and placenta are handed over to the relatives after delivery.
Thus using umbilical cord for studies became difficult and this is a major
drawback in our environment considering the high perinatal and infant
morbidities and mortalities4.
The length of the
umbilical cord ranges from no cord (Acordia) to 300cm
with a diameter of 1.2cm-3.0cm5. At term the average length of the
umbilical cord is between 55cm – 60cm and with a diameter of 2.0cm -2.5cm6.
Umbilical cord
shorter than 35cm occurs in 5-6% of cases and in about 5-6% of cases the
umbilical cord length is longer than 80cm7. Though what controls the
umbilical cord length is not fully understood, however various authors ascribed
cord length to be due to fetal activity and movement8.
A short umbilical
cord is defined as an umbilical cord length less than 30cm and it occurs in
5-6% of pregnancies. The pathogenesis of short cord remains unclear,
however stretch hypothesis explains the ontogeny of the umbilical cord9.
Short cords have been associated with ante-partum and intra-partum
complications and occur commonly in female neonates10
An umbilical cord
longer than 70cm are said to be long and they also occur in 5-6% of pregnancies10.
The complications of long umbilical length could be maternal and fetal and
there ranges from cord entanglement, fetal anomalies, mal-presentation, macrosomia and respiratory distress. Long umbilical cords
are commonly seen in male neonates.
In investigating the
clinical significant of umbilical cord length, it was found that the umbilical
cord length was significantly correlated to fetal outcome, however, various
studies has conflicting reports on this issue hence the aim of this study is to
determine the relationship between fetal umbilical cord length and fetal
outcome in our centre.
The importance of
umbilical cord length abnormalities have been under-estimated with its
attendant obstetric complications contributing significantly to the high
perinatal and infant morbidities and mortalities11.
Different
characteristics of umbilical cord
structure and function may predispose a given fetus to umbilical cord accident12,
These umbilical cord
characteristics include cord length, cord weight, cord tensile
strength, cord circumference, cord diameter and whatons
jelly content13. The umbilical cord length is the only property of the
umbilical cord which is associated and documented as a definite risk factor for poor fetal outcome14,
Other umbilical cord properties are linked to the umbilical cord length, hence
umbilical cord length abnormalities contribute significantly to umbilical cord
accident15. Umbilical cord accident has an
incidence of 1.5 stillbirth per
1000 birth16. Umbilical cord
accident also accounts for 15 percent of
all sudden antenatal death syndrome17,18. Sudden antenatal death
syndrome accounts for 30,000 fetal death per year19
.The reviews of singleton birth files showed that umbilical cord accident
accounts for 3.6 death per 1000 births excluding congenital malformations20.
The best evidence report published as at the year 2002, umbilical cord accident
accounts for 2 fetal death per 1000 births and this translates to 4000 to 8000
death per year of genetically normal fetuses in the United states of America21.
The burden of abnormal cord length on the nation cannot be over emphasized,
The result of this
study will highlight the clinical importance of umbilical cord length in our centre. The study will give room for other studies that will
measure umbilical cord prenatally and evaluate the risk factors of umbilical cord length for poor fetal outcome.
Furthermore, the
measurement of umbilical cord length to detect abnormality in umbilical cord
length and relationship with fetal outcome in our centre, will encourage more
studies to identify modifiable causes of abnormal umbilical cord length hence
improving fetal outcome.
Therefore, I will
replicate this study in our center since it has not been carried out and
compare the result from other studies,.
Aim
The aim of this study was to determine the
correlation between the fetal umbilical length and the fetal outcome.
The Specific
Objectives are:
·
To determine the mean fetal umbilical cord
length and normal fetal umbilical cord length among parturients
who delivered at term in FMC Owerri.
·
To compare the fetal outcome between short
umbilical cord and long umbilical cord length on term babies delivered at FMC Owerri.
·
To compare the fetal outcome between long
umbilical cord and normal umbilical cord length on term babies delivered at FMC
owerri.
·
To compare the fetal outcome between short
umbilical cord length and normal umbilical cord length on term babies delivered
at FMC owerri.
·
To determine the prevalence of cord
complication in abnormal and normal cord lengths on term babies delivered at
FMC Owerri.
·
To determine the association between cord
status (normal/abnormal) and cord Complications on term babies delivered
at FMC Owerri.
Hypotheses
·
There is no relationship between fetal
umbilical cord length and fetal outcome
·
Cord status is not associated with cord
complications
·
The developing fetus or embryo is connected
to the placenta through the umbilical cord.
The most important
part of the feto-placenta unit is the umbilical cord22.,Umbilical cord length abnormalities constitute
significantly to perinatal morbidities and mortalities. The length of the
umbilical cord at term varies from absent cord to a length up to 300 centimeter23.
At birth the average length ofthe umbilical cord is
about 50-60 centimeters and a diameter of 12 milimeter24. Through the
pathology of the variability of the umbilical cord length remains unknown 25.
There are few
documented studies on the correlation between fetal umbilical cord length and
fetal outcome. The paucity of information on this subject may be due to the
fact that it is not a common practice in most centers to examine or measure
umbilical cord length after delivery of the fetus unlike the placenta which is
examined after delivery.
In a study of 1000
deliveries in India, the umbilical cord length varies from 24 centimeters to
124 centimeters. In this study the mean cord length was 63.86 centimeters (+
15.69 centimeters). The maximum cases were seen in the group of umbilical cord
length between 51 centimeters and 60 centimeters the lower 5th
percentile was considered as short umbilical cord and upper 5th
percentile was considered as long umbilical cord. Short and long umbilical
cords were associated with significant incidence of lower segment caesarean
section. Umbilical cord length did not vary according to the fetal weight, baby
length and sex of the newborn. This study concluded that umbilical cord length
abnormality had higher incidence of cord complication, increased incidence of
operative interference, intra-partum complication and consequently birth
asphyxia26.
In another
study of 200 cases on the relationship between umbilical cord length with fetal
and maternal outcome. This study used 100 cases in the control
group and the study group comprising of 20 cases of short umbilical cord length
and 80 cases of long umbilical cord length. The minimal observed cord length
was 28 centimeter and the maximum cord length was 198 centimeters and the
average umbilical cord length was 53.7 centimeters. The study concluded that
the umbilical cord length was associated with poor APGAR
score and that the umbilical cord length in relation to the sex of the fetus
was insignificant27.
In a study carried
out in Japan on the correlation between the length of the umbilical cord and
perinatal outcome. This study showed that the average length of the umbilical
cord was 56.2 + 11.70 centimeters (range 19-133 centimeters). Long
umbilical cord was defined as those umbilical cord measuring approximately +
1.5 SD above the mean and short umbilical cord length measuring – 1.5 SD below
the mean. The mean are >74 and < 38 centimeter in length. Normal
cord length was defined as those umbilical lengths measuring + 1.0 SD of
the mean which is 45 – 68 centimeters in length. The study showed that short
umbilical cord length was associated with increased rate of emergency caesarean
section, while long umbilical cord was associated with multiple nuchal cords
and umbilical knots.
However, this study
concluded that umbilical cord length abnormality might not be associated with
adverse perinatal outcome in Japan28. In another study of 500 cases
in India, the study showed that the umbilical cord length varies from 24-124
centimeters and the mean umbilical cord length was 61.7 centimeters. The
maximum cord length was observed in the group of cord length between 61 and 70
centimeters. Lower 5th percentile was considered as short umbilical
cord and upper 5th percentile was considered as long umbilical cord.
The study concluded that fetal umbilical cord length did not vary according to
the fetal weight, fetal length and sex of the fetus29.
In a study
of 531 cases on the correlation between umbilical cord length and intra-partum
complication. The umbilical cord length varies from 14 to 129
centimeters and the mean umbilical cord length was 58 centimeters. The study
defined short umbilical cord length as umbilical cord length of 35 centimeter
or less (lower 6th percentile). The study also showed that umbilical
cord accidents were more frequent in long umbilical cord; the study further
stated that abnormal cord length was associated with abnormal fetal heart
pattern30.
A prospective,
population based
cohort study. The study involved 11,580 individual born between
1915 -1929 in Uppsala Sweden, there were 135 patient with chronic rheumatic
heart disease (72 men and 64 women) with a mean age of first hospital admission
of 68yrs (range 36-92). There was evidence of a positive association between
umbilical cord length and risk of subsequent chronic rheumatic heart disease.
The overall hazard ratio in the Sweden study (1.13: 95% confidence interval
1.01 to 1.27) was similar to the previous study with some suggestion of larger
effect in men than in women, however there was no other birth characteristics
that was predictive except for weak
evidence of a protective effect of higher birth weight in men31.
In a study
of the relationship between umbilical cord length and chronic rhematie disease in Sweden. This study was a
prospective cohort study and it showed that there was a positive association
between umbilical cord length and the risk of subsequent chronic heart disease32.
In a study of 1000
deliveries in South eastern Nigeria, the study showed
that the mean umbilical cord length was 51.5 centimeters. The study further
showed that there was a significant correlation of the fetal umbilical cord
length with both the fetal weight and placenta weight33.
In another Nigerian
study of 602 cases, study showed the average umbilical cord length was 57.56cm
and the fetal outcome was not discussed34.
Another
Nigerian study of 305 cases in South Western Nigeria in the study of the
correlation between umbilical cord length with baby length and weight. The study
showed that the minimum umbilical cord length was 29.5 centimeters and the
maximum cord length in this study was 100 centimeter the mean umbilical cord
length was 51.5 centimeter + 6.67 centimeters. In this study there was
positive correlation between umbilical cord length and the length of the baby
and there was also positive correlation between the umbilical cord length and
the weight of the fetus35.
Umbilical cord in
35,779 neonates was analysed to determine values
after mid gestation and to see if abnormal values have clinical significance.
Growth slowed after 28 weeks of gestation but did not stop before term. Cord
length had a positive correlation with maternal height, weight, pregnancy
weight gain, socio-economic statue and the fetus
being male.
Short cords were
associated with subsequent psychomotor abnormalities, but taken alone their
predictive value was low because the normal range of cord length was large.
Short cords were much better predictors of subsequent impairment when they were
combined with other neonatal predictors. Short cords doubled or tripled the
predictive values of low APGAR scores and several other neonatal abnormalities
for subsequent low IQ values and neurologic abnormalities36.
Another study
investigated eight healthy term infants with short umbilical cord and 15
control term infants, mothers with pre-eclampsia or
hypertension, chorioamnionitis or prolonged rupture
of membrane were excluded from the study maternal birth weight, age, parity,
infant gender and placenta weight were
recorded. The umbilical cord length and diameter were measured as well as the newborn tubal Speed
of Sound (SOS). SOS measurement (simlight
Omensense 7000P instrument) were obtained at
the tubal mid shaft.
The study shows that
there were no difference between the two groups in the mother age, parity,
newborn’s gender, birth weight or placenta weight, however, infant with short
umbilical cord length had lower bone (SOS) measure their infant with normal
cord length 3047 + 107 m/sec vs 3194+
311 m/sec, (p<0.05). The newborn’s (SOS) was correlated only with the
umbilical cord length (R = 0.57, p = 0.008) and not with maternal age, infant
gender, placenta weight, umbilical cord diameter.
The study concluded
that infants with short umbilical cord have a lower tibia SOS measurement
compared with infant’s normal length cord and this finding is likely due to
decrease level of activity37.
In the review of
these few documented studies,
it was observed the length of the umbilical cord varies. it was also observed
that on the correlation between fetal umbilical cord
length and fetal outcome. that some Authors agreed that there was a positive
correlation between fetal umbilical cord length and the fetal outcome, while
some authors denied this correlation. However, in the mist of this conflicting
reports on this subject. It was observed that umbilical cord length abnormality
was associated with various umbilical cord complications which will have
significant impact on the perinatal morbidities and mortalities.
Umbilical cord length
abnormalities are involved in fetal and neonatal complication. Abnormal
umbilical cord length have been recognized as the most
important umbilical cord features linked to unfavourable
results38.
The knowledge of the
length of the umbilical cord is quite useful in the physio-pathological
interpretation of the placenta index39. It is also of interest to
measure the length of the umbilical cord to predict dystocia and other
challenges related to umbilical cord length abnormalities. However accurate
measurement of the total length of the umbilical cord is a challenge.
Few authors have
tried to explain how to measure the total length of the umbilical cord, but the
results were not reliable because landmarks were not used in the measurement
In a study of 1000
deliveries, the umbilical cord was clamped at two places and cut in between.
Then from the cord end, up to the fetal umbilical and the placenta attachment,
the umbilical cord length was measured and added, this measurement was done
with a flexible tape in centimeters. Landmark was not used in this study and
the results of these measurements may vary from one individual to
another.
In another study the
umbilical cord was clamped at the maternal introitus
immediately after delivery of the neonates, the umbilical cord segment was
measured from the introitus to the placenta
attachment40.
An
observational analytic study to describe measurement of the umbilical cord
length.
In this study 20.3 centimeter pair of curved Rochester classic forceps were
lain on the top of the umbilical cord with the handle placed against the
abdomen of the neonate; then
first clamp was made at a distance of 20.3 centimeter. Thereafter
moving towards the body of the newborn, another clamp was made at 20.3
centimeter. The rest of the umbilical cord attached to the placenta was measured, thereafter 20.3 centimeter was added to give the
total length of the umbilical cord41. Though the author believed
that the measurement of the umbilical cord length through this method was
simple but it seems complex and besides the addition of 20.3 centimeter made
the measurement ambiguous.
In another Nigerian
study; the measurement of the fetal umbilical cord length was carried out
immediately after delivery of the neonate. The umbilical cord was clamped at 5
centimeters from the abdomen of the neonate and after cutting in between
clamps, the neonate was handed over to the pediatrician for APGAR scoring and
immediately after the removal of the placenta the length of the umbilical cord
was measured using a flexible tape. The length of the cut end attached to the
fetus was added to the length of the umbilical cord attached to the placenta
and this gave the total length of the umbilical cord. This method is simple and
it is also the landmark
recommended by the paediatricians hence
in this study this landmark will be used.
Study
Design
This was a cross sectional study involving
eligible parturients at term. The women were recruited consecutively
and after counseling them in respect to this study, their informed consent to
participate was sought. Those who
consented were
enrolled and data sheet completed by the researcher. The data sheet contained the Name of patient, Age, Marital status,
Religion, Tribe, Occupation, Obstetric history, Medical and social history, Labour history, Umbilical cord examination, Newborn
parameters.
Study Area
The study was carried out at the Federal Medical
Centre, Owerri, Imo State, South Eastern Nigeria. It
is a tertiary Health Institution undertaking postgraduate medical training. The
hospital is located in Owerri Metropolis the capital
of Imo State with a population of about 500,000 people and estimated 140,000
(28%) of these are women of reproductive age. The hospital serves as a referral
centre for both government and private health
facilities for Imo State. The inhabitants of Owerri
and its environs are mainly Igbos and other migrant workers mainly civil
servants, traders and subsistence farmers. Most of the people are Christian by
religion and few Muslims and pagans are found. The hospital provides all levels
of health care services for Imo State and neighbouring
parts of Rivers, Abia and Anambra
States.
The study subjects were drawn from antenatal
clinics, prenatal wards and labour ward of the
hospital. The antenatal clinics hold every working day in a week. An average of 250 neonates are delivered per month and 5250
per year in the hospital.
Training
of Assistants
Two registrars were trained to assist the researcher in
carry out this study. The registrars underwent two weeks training and after which they assisted
the researcher in the study This
was to ensure accuracy of data
collection.
Recruitment
of parturients
All parturients at
term who met the inclusion criteria after completion of the data sheet were enrolled
consecutively for the study until a sample size of 427 was obtained. The study was completed in 3
months.
Inclusion
Criteria
All parturients at
term in labour
Singleton fetus
Exclusion
criteria
Parturients
in preterm labour.
Parturients
with retroviral disease, diabetes mellitus, hypertensive disease of pregnancy,
Intra-uterine Growth Restriction (IUGR).
Parturients
whose fetuses have congenital malformation.
Calculation
of the sample size
A sample size was selected to detect the mean cord
length and correlation between the umbilical cord length and the fetal weight
at 95% confidence level and a standard deviation of 0.05. the probability of
achieving statistical significant with power of analysis was based on previous
study of three hundred and five (305) parturient, the average birth weight 3.23+0.50
kilogram and the average cord length was 50.50+SD 6.67 centimeter (There
was a significant positive correlation between cord length and fetal weight) (r
= 0.145, p = 0.011)34. Thus using the formula42
for sample size in a correlation studies for continuous outcomes.
Sample size

Z1-α/2
= standard normal value = 1.96,
σ=
standard deviation of babies weight from previous study = 0.5kg
d = precision
error = 5% or 0.05
Hence the
sample size n is calculated as follows:

 =
= 
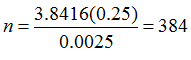
To account for 10% attrition , we now have n=  =427
=427
METHODOLOGY
Parturients at term
who met the eligibility criteria were admitted in labor ward. Obstetric
examination was
carried out to confirm their gestational age, the lie,
presentation, position, descent of the presenting part and the fetal heart rate
will be auscultated with the pinard stethoscope.
Vaginal examination was
carried out to ascertain the state of the cervix, the dilatation
of the cervix, the state of the membrane, the presenting part, the station of
the presenting part. The presence or otherwise of caput or moulding
were also be
noted.
Parturients who were in active phase
of labour would
be admitted to the partograph and their labour managed partographically
until they had the urge to bear down.
Then they were
encouraged to bear down with each contraction. At the delivery of
the baby, third stage was
managed actively.
At the delivery of
the newborn the following observations regarding the umbilical cord were looked out for: the presence or otherwise of loop around the neck or
shoulder, cord loops tight or loose, number of loops of cord, position, knots
of cord (true or false), cord abnormalities, cysts, haematoma.
After delivery of the
newborn, the umbilical cord was double clamped at 5 centimeter from
the umbilicus and cut in between. Then from the cut end up to the fetal
umbilicus was measured
and added to the length of the cord from the cut end up to its placental
attachment. The sum gave
the total length of the umbilical cord. It was measured with a flexible tape in
centimeters. The flexible tapes were bought from same company to ensure
equal calibration of the tape rules. The number of umbilical arteries, coiling
index were not
be studied. Also the type of insertion of the placenta was not
noted. The following parameters were recorded after delivery:
The AGPAR scores at 1minute and 5 minutes
The weight of the newborn
The umbilical cord length
Number of umbilical loop around the neck
Number of umbilical knots
Birth length.
Data
analysis
Statistical analysis was carried out using
statistical package for the social science (SPSS) version 23. Student t-test
was used for continuous variables while Chi-square was,done for contiguous variables. Microsoft excel and Pearson correlation were
carried out using
SPSS. All charts were drawn with Microsoft Excel, statistical significance was
defined as p<0.05.
Dissemination
of result
The result of this study would be submitted
to the National Postgraduate Medical College as a partial fulfillment of the
requirement for the Part II Fellowship examination of the Faculty of Obstetrics
and Gynecology. Relevant sections will in due course be presented in scientific
conferences and be published in peer review journals.
Limitation for the
Study
There are few documented studies on this
subject.
Standardization
of measuring the total umbilical cord length. There has not been a
standard method of measuring the total length of the umbilical cord from
previous studies.
Inter-observer error
The
Strength of the Study
The strength of this study lies on the
following:
The sample size.
The measurement of the fetal umbilical cord was measured twice to
ensure accuracy.
The data would be reliable since the
measurement was taken
immediately after delivery
RESULTS
4.1 Socio-Demographic Characteristics of the
Subjects, Mode of Delivery and Cord Length. Among the women used in the study,
the oldest ones were at age 43years while the youngest was 18 years old. Only 4
women were less than 21 and all of them delivered babies with normal cord
length. More than half of the mothers (235 or 54.0%) were between 21- 30 years of
age, of which clear majority(90.6%) gave birth to children with normal cord
length, 3 (1.3%) gave birth to children with short cord length while 7(3%)
delivered babies with long cord length (Table1). Among the mothers whose age at birth were over 41 years, None delivered an abnormal
(long) cord length child. However, statistical test indicates that there values
are likely to have occurred by chance since there was no significant evidence
of association between mothers’ age at birth and the birth cord length of a
child in this study (p=0.987, χ2
=2,386).
At parity
of 1, there were 3 (2.1%) short cord lengths and 7(5%), long cord lengths.
Parity 2-3 children showed 1 (0.5%) short cord length and 8 (3.9%) long cord
length. At parity of more than 5 children, 1 (20%) long cord length was found.
Clearly no evidence of statistical association was established between parity
and cord length status in this study (p =0.136, χ2 =9.744). Almost all the women studied were married with just a single mother
(0.2%). The single mother delivered a baby with normal cord length. No evidence
of significant association was found between marital status and cord
length in this study (p =0.975, χ2 =0.051).
Those who
were unbooked were 3 (0.69%), and 2 (66.7%) showed
normal cord length and 1 (33.3%) had long cord length. For the booked, 1.2% have short cord length,
88.7% normal and 10.2% long. Booking status
was not found as a significant associating factor of cord length status. The
subjects were mainly Ibos (98.2%), with 3 (0.69%) and 1 (0.23%) respectively of
Yoruba and Hausa tribes. There were also 4 (0.92%) other women from other
tribes such as Ibibio, Efik and Tiv.
Among the Ibos, 5 (0.9%) were of short cord length, 378 (88.8%) were normal and
44 (10.3%) were long. None of the babies from Hausa and Yoruba tribe showed
abnormal cord length while only 1(25%) long cord length was observed among
other tribe. Tribe was not found as a significant factor in this study (p =0.494,
χ2 =5.398), indicating
that some few observed difference in cord length among different tribes may
have occurred by chance.
In terms
of religion, the study participants were predominantly Christians (99.8%) with
only 1 (0.2%) Islam, all the abnormal cord length were found in the Christians,
but religion was not found as a significant associating factor of cord length
status in this study (p =0.975, χ2 =0.051).
In terms
of mode of delivery, 292 (67%) babies were delivered by spontaneous vaginal
delivery (SVD), followed by 92 (2.1%) on emergency cesarean section and 42
(9.7%) on elective cesarean section. Up to 8 (1.8%) were delivered on vacuum
delivery while 1 (0.2%) was through breech delivery. The association between
cord length and the mode of delivery, as well as the association between Cord
length and the sex of the baby were also computed
(Table 8). For delivery mode, a total of 292 babies were born on Spontaneous vaginal delivery (SVD), 3 (1.0%) had short cord length,
258 988.4%) had normal cord length and 31 (10.6%) had long cord length. Among
92 babies delivered with emergency cesarean section, 2 (2.2%) had short cord
length and 8 (8.7%) had long cord length. For the babies delivered born on
elective cesarean section, 6 (14.3%) had long cord length and the remaining 36
(85.7%) were of normal cord length. A total of 8 babies were delivered through
vacuum delivery and all of them showed normal cord length. Only one baby was
delivered by breech and the baby also showed normal cord length. Statistical test
indicates that there was no evidence of association between mode of delivery
and cord length (p=0.913,
χ2 =3.314).
Table 1: Distribution for Demographic characteristics
and Mode of delivery
|
Demographic
characteristics and Mode of delivery
|
Total
|
Short
|
Normal
|
Long
|
Chi-square
|
p-value
|
|
|
|
N
|
%
|
N
|
%
|
n
|
%
|
(χ2)
|
(p)
|
|
Mother’ Age (in yrs)
mean =30.30 (±4.51)
|
|
|
|
|
|
|
|
|
|
|
less than 21
|
4
|
0
|
0.0
|
4
|
100
|
0
|
0.0
|
|
|
|
21- 30
|
235
|
3
|
1.3
|
213
|
90.6
|
19
|
8.1
|
|
|
|
31 -35
|
140
|
1
|
0.7
|
119
|
85.0
|
20
|
14.3
|
|
|
|
36-40
|
47
|
1
|
2.1
|
41
|
87.2
|
5
|
10.6
|
|
|
|
41+
|
9
|
0
|
0.0
|
8
|
88.9
|
1
|
11.1
|
|
|
|
Total
|
435
|
5
|
1.1
|
385
|
88.5
|
45
|
10.3
|
2.366
|
0.968
|
|
Parity
|
|
|
|
|
|
|
|
|
|
|
1
|
140
|
3
|
2.1
|
124
|
88.6
|
13
|
9.3
|
|
|
|
2 -3
|
206
|
1
|
0.5
|
183
|
88.8
|
22
|
10.7
|
|
|
|
4-5
|
84
|
1
|
1.2
|
74
|
88.1
|
9
|
10.7
|
|
|
|
>5
|
5
|
0
|
0.0
|
4
|
80.0
|
1
|
20.0
|
|
|
|
Total
|
435
|
5
|
1.1
|
385
|
88.5
|
45
|
10.3
|
9.772
|
0.135
|
|
Marital status
|
|
|
|
|
|
|
|
|
|
|
Single
|
1
|
0
|
0.0
|
1
|
100
|
0
|
0.0
|
|
|
|
Married
|
434
|
5
|
1.2%
|
384
|
88.5%
|
45
|
10.4
|
|
|
|
Divorced
|
0
|
0
|
0.0
|
0
|
0.0
|
0
|
0.0
|
|
|
|
Total
|
435
|
5
|
1.1
|
385
|
88.5
|
45
|
10.3
|
0.051
|
0.975
|
|
Booking Status
|
|
|
|
|
|
|
|
|
|
|
Unbooked
|
3
|
0
|
0.0
|
2
|
66.7
|
1
|
33.3
|
|
|
|
Booked
|
432
|
5
|
1.2
|
383
|
88.7
|
44
|
10.2
|
|
|
|
Total
|
435
|
5
|
1.1
|
385
|
88.5
|
45
|
10.3
|
1.741
|
0.419
|
|
Tribe
|
|
|
|
|
|
|
|
|
|
|
Igbo
|
427
|
5
|
0.9
|
378
|
88.8
|
44
|
10.3
|
|
|
|
Hausa
|
1
|
0
|
0.0
|
1
|
100
|
0
|
0.0
|
|
|
|
Yoruba
|
3
|
0
|
0.0
|
3
|
100
|
0
|
0.0
|
|
|
|
Others
|
4
|
0
|
0.0
|
3
|
75.0
|
1
|
25.0
|
|
|
|
Total
|
435
|
5
|
1.1
|
385
|
88.5
|
45
|
10.3
|
5.398
|
0.494
|
|
Religion
|
|
|
|
|
|
|
|
|
|
|
Christianity
|
434
|
5
|
1.2
|
384
|
88.5
|
45
|
10.4
|
|
|
|
Islam
|
1
|
0
|
0.0
|
1
|
100
|
0
|
0.0
|
|
|
|
Traditional
|
0
|
0
|
0.0
|
0
|
0.0
|
0
|
0.0
|
|
|
|
Total
|
435
|
5
|
1.1
|
385
|
88.5
|
45
|
10.3
|
0.051
|
0.975
|
|
Mode of Delivery
|
|
|
|
|
|
|
|
|
|
|
Spontaneous vaginal delivery
(SVD)
|
292
|
3
|
1.0
|
258
|
88.4
|
31
|
10.6
|
|
|
|
Emergency cesarean section
|
92
|
2
|
2.2
|
82
|
89.1
|
8
|
8.7
|
|
|
|
Elective cesarean section
|
42
|
0
|
0.0
|
36
|
85.7
|
6
|
14.3
|
|
|
|
Vacuum delivery
|
8
|
0
|
0.0
|
8
|
100.0
|
0
|
0.0
|
|
|
|
Breech delivery
|
1
|
0
|
0.0
|
1
|
100.0
|
0
|
0.0
|
|
|
|
Total
|
435
|
5
|
1.1%
|
385
|
88.5%
|
45
|
10.3
|
3.314
|
0.913
|
Mean Fetal umbilical cord Length and other
Fetal Outcomes
There were a total of 435 deliveries studied.
Clearly the mean cord length obtained in the study for the babies was 60.35cm,
at a corresponding standard deviation of 10.39. The shortest cord length among
the babies was 33cm while the longest one was 120cm (Table 2).The normal fetal
umbilical cord length in this study is the mean fetal umbilical cord length _+
2SD,Which is 60.35cm _+20.78, Therefore a short fetal
umbilical cord length is defined as a fetal umbilical cord less than
39.5cm,however,the normal fetal umbilical cord length ranges between 39.5cm to
81.1cm.A long fetal umbilical cord length is defined as an umbilical cord
length longer than 81,1cm.
Also
Table 2 contained summary information on other fetal outcomes such as birth
weight, birth length, gestational age and APGAR scores at 1 minute and 5
minutes. The mean birth weight was 3.20kg (Standard deviation = 1.47 kg). The
minimum and maximum birth weight obtained were 1.85kg and 5.30kg respectively.
On the other hand, the mean birth length was 49.5 cm at a standard deviation of
2.87cm. The shortest birth length was 33cm and the longest 60cm.
The
mean gestational age was 39 weeks at a corresponding standard deviation of 1.14
weeks). At I minute APGAR
score, a mean (± standard deviation) score of 8.1 (± 1.10) was
obtained, with minimum and maximum scores of 3.0 and 10.0 respectively. The mean (±standard deviation) APGAR score of
9.8 (± 0.80) was obtained at 5 minutes, with minimum score of 4 and maximum
score of 10.
Table 2: Mean Fetal umbilical cord Length and
other Fetal Outcomes
|
Fetal Outcomes
|
n
|
Minimum
|
Maximum
|
Mean
|
Std. Deviation
|
|
Cord
Length (cm
|
435
|
33.00
|
120.00
|
60.35
|
10.39
|
|
Birth
Weight (kg)
|
435
|
1.85
|
5.3
|
3.20
|
0.49
|
|
Birth
Length (cm)
|
435
|
33.00
|
60.00
|
49.50
|
2.87
|
|
Gestational Age (Weeks)
|
435
|
35.00
|
44.00
|
39.0
|
1.14
|
|
APGAR
score (1 min)
|
435
|
3.00
|
10.00
|
8.11
|
1.10
|
|
APGAR
Score (5 mins)
|
435
|
4.00
|
10.00
|
9.75
|
0.80
|
Length
of Umbilical Cord Case Distributions
The output contained on Table 3
is the case distribution according to the cord length for the babies studied. The
distribution was such that clear majority 95.16% of the children have normal
cord length (39.5-81.1cm) while 3.69%
showed long umbilical cord length (> 81.1cm) and 1.15% was short umbilical
cord lengths (< 39.5cm). Hence, the
total abnormal cord length (short and long) found in this study was 21 (4.84%).
Table
3: Case distribution according to length of cord
|
Length of Cord
|
Number of cases (n)
|
Percent (%)
|
|
Short cord
|
5
|
1.15
|
|
Normal cord
|
414
|
95.17
|
|
Long cord
|
16
|
3.68
|
|
Total
|
435
|
100
|
4.4
Correlation between Fetal umbilical Cord Length and other Fetal
outcomes
Table 4 contained the
summary statistics of fetal outcomes in relation to the cord length. The
overall correlation between birth weight and cord length was found to be
positive but poor (r =0.244). The correlation was positive in the normal and
long cord lengths but negative in the short cord length (r =-0.4289).
Significant association was established between cord length and birth
weight in this study (p < 0.0001).
On
sex of the baby, none of the male babies showed short cord length at birth
while 10 (4.4%) and 220 (95.7%) had long cord length and normal cord length
respectively. For the females, 5 (2.5%) had short cord length, 188(95.7%) had
normal cord length and 6 (3.0%) had long cord length. Slight significant
association was found between baby sex and cord length (p =0.048,χ2=6.028).
At one minute APGAR score, the overall correlation was quite very poor (r
=0.008). Poor positive correlation were obtained in short (r =0.333)
and normal (r =0.034) cord length while it
negative at long cord length (r = -0.156). Similar poor correlations were obtained at 5
minutes APGAR score for short (r = 0.000), normal (r = 0.062) and long (r = -0.0) cord lengths. However, no
significant association was found between cord length and APGAR scores in both one and five minutes.
Overall poor positive
correlation was obtained between birth length and cord length (r = 0.256). The correlations were positive in the normal cord
length (r = 0.219) and long cord length (r = 0.378), but negative in the short cord length (r = -0.230). Significant positive correlation was obtained in
between birth length and cord length (p< 0.0001). The correlations for
gestational age were r= 0.589 in short cord length, r= -0.0175 in normal cord
length and r= 0.354 in the long cord length; but no evidence of significant
association was found between cord length and gestational age in this study (p
= 0.875).
4.5 Correlations between Fetal Cord Length
and other Fetal outcome
Table 3 contained the
summary statistics of fetal outcomes in relation to the cord length. There were
poor correlations found between birth length and different cord lengths. The
correlation was positive between birth length and the normal cord length
(r=0.219) and between birth length with long cord length (r=0.378), but was
negative between birth length with short cord length (r=0.230).
In terms of
correlation between birth weight and cord lengths, the correlation was positive
with normal cord length (0.084), and long cord lengths (0.2467) but negative in
the short cord length (r=0.0074). For the APGAR score, poor positive correlation were
obtained between APGAR score and short
fetal cord length (r=0.333), as well as between APGAR score and normal cord
length (r=0.034).
Table 4:
Correlation between feotal Cord Length and other
Fetal Outcome
|
Outcome
|
Short
umbilical cord (n=5)
|
Normal
umbilical cord (n=414)
|
Long
umbilical cord (n=16)
|
|
Birth length (cm)
|
-0.230
|
0.219
|
0.378
|
|
Birth weight (kg)
|
-0.0074
|
0.084
|
0.2467
|
|
APGAR
score
|
0.333
|
0.034
|
-0.156
|
On table 4a, the mean
birth weight showed some evidence of significant difference between short and
long umbilical cord lengths (p=0.0442, t=-2.1556), with means of 3.08kg and
3.58kg respectively in short and long umbilical cord lengths. The mean birth
length was found to be 48.2cm (standard deviation = 2.05) at short umbilical
cord length, while it was 51cm (standard deviation =3.03) at long umbilical
cord. The mean Apgar score was respectively 9.0 and 8.0 at short and long cord
lengths. Statistical test shows that no significant difference was found
between short and long umbilical cord lengths in relation to birth length (t=-1.9163,p=0.0705) and APGAR score (t=1.6863,p=0.1081).
Birth length was
found to be slightly significant between long and normal umbilical cord lengths
(t=2.0446,p=0.0415), at a mean value of 51.0cm and
49.46cm respectively for the long and normal cord lengths. None of the birth
weight (t=0.8563,p=0.3923), and APGAR score (t=-0.2865,p=0.7746) was found
significant between long and normal cord lengths in this study.
The result for the
relationship between short and normal umbilical cord lengths in terms of feotal outcomes such as birth length, birth weight and
Apgar score is also contained on Table 4c. No statistical significant
difference was found between the two different umbilical cord lengths at any of
the fetal outcomes
at 5% level.
Table 4a:
Relation between feotal cord length and other fetal
outcomes comparing fetaloutcome between Short
umbilical cord length and Long umbilical cord length
|
Outcomes
|
Mean +
standard deviation
|
Mean +
standard deviation
|
t test
|
P value
(p)
|
|
|
Short umbilical cord (n=5)
|
Long umbilical cord (n=16)
|
|
|
|
Birth length (cm)
|
48.2+2.05
|
51.0 + 3.03
|
-1.9163
|
0.0705
|
|
Birth weight (kg)
|
3.08 + 0.19
|
3.58 + 0.50
|
-2.1556
|
0.0442
|
|
Apgar score
|
9.0+ 0.71
|
8.0+ 1.25
|
1.6863
|
0.1081
|
Table 4b:
Relation between fetal cord length and other fetal outcomes comparing fetaloutcome between long umbilical cord length and normal
umbilical cord length
|
Outcomes
|
Mean +
standard deviation
|
Mean +
standard deviation
|
t test
|
P value
(p)
|
|
|
Short umbilical cord (n=16)
|
Long umbilical cord (n=414)
|
|
|
|
Birth length (cm)
|
51.0+3.03
|
49.46 + 2.86
|
2.0446
|
0.0415
|
|
Birth weight (kg)
|
3.58 + 0.50
|
3.26 + 1.49
|
0.8563
|
0.3923
|
|
Apgar score
|
8.0+ 1.25
|
8.08+ 1.09
|
-0.2865
|
0.7746
|
Table 4c:
Relation between fetal cord length and other fetal outcomes comparing foetal outcome between Short umbilical cord length and
normal umbilical cord length
|
Outcomes
|
Mean +
standard deviation
|
Mean +
standard deviation
|
t test
|
P value
(p)
|
|
|
Short umbilical cord (n=5)
|
Long umbilical cord (n=414)
|
|
|
|
Birth length (cm)
|
48.2+2.05
|
49.46 + 2.86
|
-0.9815
|
0.3269
|
|
Birth weight (kg)
|
3.08 + 0.19
|
3. 26 + 1.49
|
-0.2698
|
0.7875
|
|
Apgar score
|
9.0+ 0.71
|
8.08+ 1.09
|
1.8812
|
0.0606
|
4.5
Prevalence of Cord Complications in the Overall, Normal and Abnormal Cord
Lengths
Among
the group studied, 16 (3.7%) have cord complication while 419 (98.4%) do not
have cord complications. Hence the oveall prevalence of cord complications was
found as 3.7% in this study (Table 5).
Among 21 babies that
showed abnormal cord length, 4 (19%) had cord complications while 17 (81%) were
without cord complications. For the ones with short cord length, 20% have
complication, and for those with long cord length, 18.7% have complications while
for the babies that have normal cord length, only 2.9% have complications
(Table 5).
Clearly the
prevalence of cord complications was found to be higher in babies with abnormal
cord length than in the ones with normal cord length. The difference in prevalence between the
abnormal and normal cord length was found to be statistically significant (p< 0.0001, χ2
=13.35).
Table 5:
Prevalence of Cord Complications in Normal and Abnormal cord length
|
Cord length
|
Number
|
(Prevalence)
|
|
Short Cord length
|
|
|
|
Complications
|
1
|
20%
|
|
Non-complications
|
4
|
80%
|
|
Total
|
5
|
100%
|
|
|
|
|
|
Normal Cord length
|
|
|
|
Complications
|
12
|
2.9%
|
|
Non-complications
|
402
|
97.1%
|
|
Total
|
414
|
100%
|
|
|
|
|
|
Long Cord length
|
|
|
|
Complications
|
3
|
18.7%
|
|
Non-complications
|
13
|
81.3%
|
|
Total
|
16
|
100%
|
|
|
|
|
|
Overall
|
|
|
|
Complications
|
16
|
3.7%
|
|
Non-complications
|
419
|
96.3%
|
|
Total
|
435
|
100%
|
|
|
|
|
|
Statistical Test
|
|
|
|
p-value (p)
|
|
< 0.0001
|
|
Chi-square value (χ2)
|
|
13.35
|
4.7 Cord Complication
Status
Clearly
there were a total of 16 (3.7%) babies that had cord complications Figure 1.
The frequency of the complications was such that 10 out of the 16 complications
(62.5%) were nuchal cord with one loop and 2 (12.5%) were nuchal cord with
two loops. The rest including severe asphyxia occurred only in one baby (6.3%) each (Figure 2).

Figure 1:
Cord Complication Status

Figure 2:
Distribution for different Cord complication among the Study Population
4.8
Association between cord length status and cord complication status
Among the babies born without cord
complications, 17 (4.1%) had abnormal cord length. Similarly, for the babies
that had cord complications. nuchal cord with one loop
, 1 (10.0%) had abnormal cord length.
Two babies showed nuchal cord with two loops,
and 1 (50%) have abnormal cord length. One baby showed nuchal cord with three loops and the baby
had abnormal cord length, while one baby born with severe asphyxia had normal
cord length (Table 8). Significant association was found
in this study at 5% level, between different cord complications and cord length
status (p
< 0.006, χ2 =18.288).
Table
8: Cord length status and cord complication status
|
Cord Complication Status
|
Total
|
Normal cord length
|
Abnormal cord length
|
|
No Complication
|
419
|
402
|
95.9%
|
17
|
4.1%
|
|
nuchal cord with one loop
|
10
|
9
|
90.0%
|
1
|
10.0%
|
|
Nuchal cord
with two loops
|
2
|
1
|
50.0%
|
1
|
50.0%
|
|
nuchal cord with three loops
|
1
|
0
|
0.0%
|
1
|
100.0%
|
|
Nuchal cord with four loops
|
1
|
1
|
100.0%
|
0
|
0.0%
|
|
Nuchal cord, cord around the body and right leg
|
1
|
0
|
0.0%
|
1
|
100.0%
|
|
Severe Asphyxia
|
1
|
1
|
100.0%
|
0
|
0.0%
|
|
Total
|
435
|
414
|
95.2%
|
21
|
4.8%
|
|
|
Chi-square (χ2) =18.288
|
p=0.006
|
|
|
Further
classifications indicate that for babies born without cord
complications, 4 (1.0%) have short cord length and 13 (31.0%) have long cord
short length. For the ones born with
nuchal cord with
a loop, 10% were short cord length while none had long cord length. The babies
that have complications such as nuchal cord
with three loops and
nuchal cord together with cord around the body and right leg showed long cord
length.
DISCUSSION
The normal fetal
umbilical cord length in this study is the mean fetal umbilical cord length +
2SD, which is 60.36cm + 20.78, hence the normal
fetal umbilical cord length ranges between 39.5cm to 81.1cm. A short fetal umbilical cord length is
defined as umbilical cord length less
than 39.5cm. Also long fetal umbilical cord length is defined as an umbilical
cord length greater than 81.1cm
In this study, the
minimum fetal umbilical cord length was 33cm and the maximum cord length was
120cm. the result is not similar to the values of the umbilical cord length in
(26). The reason may be due to racial variation and even the methodology used
in the measurement of the fetal umbilical cord length. The result obtained in
this study is different from the result obtained in (27) and reason could be
due to the smaller sample size used in the study. The values obtained from (28)
are not similar to the result obtained in this study because the normal
umbilical cord length in that study was derived from mean umbilical cord length
+ 1.5 SD. It could also be due to racial variations. The result is
similar to the value obtained in (34), this could be
due to tribal similarity. Furthermore, the result obtained in this study is not
similar to the value obtained in the study (35), though same methodology was
used in measuring the fetal umbilical cord length, tribal differences could
account for the variation in the mean fetal umbilical cord length and perhaps
more female neonates were involved in that study.
The mean weight of
the neonate in this study was 3.2kg + 1.47kg which was similar to the values
obtained in (35) and the mean length of the neonate was 49.5cm + 2.87cm, which
was similar to the result obtained in (35). The reason could be due to the
methodology used in both studies and some cultural similarities in the study
population.
In
studying the relationship between fetal umbilical cord length and fetal
outcome. This study compared the relationship between long
umbilical cord length and short umbilical cord length ,
the study also compared the relationship between long umbilical cord length and
the normal umbilical cord length. The study further compared the relationship
between short umbilical cord length and normal umbilical cord length.
There was poor correlations found between birth length and
different umbilical cord length. The correlation was positive between birth
length and the normal fetal umbilical cord length (r = 0.219) and between birth
length with long fetal umbilical cord length (r=0.378), but it was negative
between birth length with short umbilical cord length (r=-0.230).
The correlation
between birth weight and different fetal umbilical cord length showed a
positive correlation between birth weight and normal umbilical cord length
(r=0.084) and long umbilical cord length (r=0.2467) but there was a negative
correlation found between birth weight and short umbilical cord length (r= -
0.0074). The correlation between APGAR
score and different umbilical cord length, showed that there was poor positive
correlation between APGAR score and short umbilical cord length (r=0.333) and
as well as between APGAR score and normal umbilical cord length (r=0.034).
In comparing the
fetal outcome between short umbilical cord length with long umbilical cord
length, it was observed that birth weight showed evidence of slightly
statistical significance (t = -2.1556, p=0.044). There was no evidence of
statistical difference of birth length (p=0.0705) and APGAR score (p- 0.1081)
respectively.
Also, when the fetal
outcome was compared between long umbilical cord and normal umbilical cord, it
was observed that the birth length was slightly statistical significant ( t = 2.0446, p=0.0415). Birth weight (t=0.8563 p= 0.3923)
and APGAR score (t = - 0.2865, p = 0.7746) were not statistically significant.
Furthermore, when the
fetal outcome was compared between short umbilical cord and normal umbilical
cord, the fetal outcome, birth length (t = - 0.9815, p = 0.3269), birth weight
(t=- 0.2698 p = 0.7875) and APGAR score
(t = 1. 8812, p = 0.0606) were not statistical significant. However there were
no previous studies that compared fetal outcome with different umbilical cord
length. The overall fetal umbilical cord length when compared with the fetal
outcome showed that
fetal umbilical cord length was statistical significant with
birth length (r = 0.256, p = <0.0001) and birth weight (r = 0.240, p =
<0.0001) but not statistically significant with APGAR score (r=0.008,p=0.875).
A recent Nigerian
study of 305 deliveries in South west Nigeria in the correlation between fetal
umbilical cord length and birth length, the mean fetal umbilical cord length
was 51.50 + 6.67cm. There was a significant correlation between fetal
umbilical cord length and birth length (35). This could result from the fact that more male babies
were involved in the study and may also result from the methodology used in
measuring the fetal umbilical cord length.
Also in another
Nigeria study of 602 deliveries in Southeast Nigeria, the mean fetal umbilical
cord length was 57.50cm. There was a positive correlation between fetal
umbilical cord length and the birth weight of the baby (34). This could result
from tribal similarity or may be that male neonate dominated in the study.
In another Nigeria
study of 1000 deliveries in Southeast Nigeria the mean fetal umbilical cord
length was 51.50cm. The study showed that there was a significant correlation
between fetal umbilical cord and fetal weight and placenta weight (33). Perhaps
tribal similarity may account for the result in the study.
In study of 500
deliveries in India, in the correlation between fetal umbilical cord and fetal
outcome, the mean fetal umbilical cord length was 61.70cm. the
lower 5th percentile was considered as short umbilical cord and the
upper 5th percentile was considered as long umbilical cord length.
The study observed the fetal umbilical cord length did not vary according to
birth weight and birth length, which is difference from what was observed in
the overall fetal umbilical cord length and fetal outcome, their reason could
be that, racial difference may have something to do with fetal umbilical cord.
In another study of 200 deliveries in Japan. In the relationship between fetal umbilical cord length and fetal
outcome. “The mean umbilical cord length was 53.70 centimeter, the study
observed that umbilical cord length was associated with poor APGAR score (27). This is not similar to
what was observed in our study, the reason could be due to racial difference
and probably the number of male neonates involved in their
study were less”.
Other important
findings in our
study were that normal umbilical cord length has a prevalence of 95.1%, the prevalence of long umbilical
cord length and short umbilical cord length were 1.15% and 3.68% respectively,
hence the prevalence of abnormal cord length in our study was 4.83%.
The other findings in
our study included that the overall prevalence of cord complication was 3.7%,
however short umbilical cord length accounted for 20%, 18.7% of the cord
complication was due to long umbilical cord length and 2.9% of the cord
complication was found in normal cord length. The difference in prevalence
between abnormal and normal cord length was statistically significant
(P<0.0001, X2 = 1.457).
There was no
relationship between maternal age, parity, marital status, booking status,
gestational age, ethnicity, religion and the mode of delivery with the overall
fetal umbilical cord length (37).
The fetal activity
and genetic constitution may have impact on the fetal umbilical cord length
development and growth. Various authors have ascribed umbilical cord length to
be due to fetal activity and movement (8). However, what controls the umbilical
cord length is not fully understood.
This study could not
determine what could be responsible for the umbilical cord length. Hence
evaluating for risk factor for abnormal cord length, identifying modifiable
causes of abnormal cord length through a multi-centred studies is recommended in order to actually
find determinants of fetal umbilical cord length thus improving fetal outcome
in our centres.
CONCLUSION
This study was primarily aimed at
investigating the relationship between fetal umbilical cord length and fetal
outcome. This aim was successfully achieved. This study showed that the length
of the fetal umbilical cord is variable. However, maximum number of cases had
normal cord length. Abnormal umbilical cord length had higher prevalence of
cord complications. There are significant positive correlations between fetal
umbilical cord length with birth weight and birth length of the baby, however,
there was no correlation found between fetal umbilical cord length and APGAR
score. The study also showed that the fetal umbilical cord length has no
correlation with maternal age, ethnicity, religion, booking statues, parity,
marital status ,gestational age, ethnicity, religion
and the mode of delivery.
Thus this study shows
the clinical importance of the fetal umbilical cord length. Examination of the feto-placenta unit after delivery will not be complete
without examining, measuring and documenting fetal umbilical cord length.
Equipment should be developed to measure the fetal umbilical cord length antenatally to reduce the prevalence of cord complications.
This will
further reduce the incidence of perinatal morbidities and mortalities
associated with cord complications in the future, thus helping to the
realization of a healthy baby at birth. Multi centered studies are required to
find the determinants
of fetal umbilical cord length.
RECOMMENDATIONS
Health education on the importance of
examination, measurement and documentation of fetal umbilical cord length after
delivery should be given to health care givers. There should be a standardize
method of measuring fetal umbilical cord length globally. There should be training and retraining
of health care providers on the accurate method of measuring fetal umbilical
cord length, Equipment should be developed
to measure umbilical cord length
during the antenatal period
,Researchers are needed in this field to evaluate risk factors and modifiable
causes of abnormal fetal umbilical cord
length. More studies are required in the new ultrasonographic
method of using umbilical cord length index to predict short or long umbilical
cord antenatally in order to improve on the
sensitivity and specificity of the method and thus improve neonatal outcome.
Ethical
Consideration
In order that ethical standards are
maintained, the following steps will be ensured. The data sheet will be
explained to eligible parturients. The parturients will be assured that no harm will result from
participating in the study. They will be made to understand that their
participation is voluntary and that their refusal to do so will not affect
their management in the hospital. They will be free to withdraw their
participation at any stage of the study.
Ethical approval will be obtained from the
hospital’s Ethical Review Committee.
Confidentiality
of data
All the information obtained from eligible
parturient will be kept strictly confidential. The patient will also be assured
that their identities will not be disclosed.
ACKNOWLEDGEMENT:
Dr Eli Sukarime MBBS,
FWACS
Executive
Director
Mother,
Baby and Adolescent Care Global Foundation (Previously Mother and Baby Care
Global Foundation) – 14/4/2021
REFERENCES
1.
Abaiclo, C. S., Boateng, K. A. and Wareen, M. A.,
Morphological Vanation of the baby’s supply line.
Journal of science and technology 2008; 28(2) 1-9.
2.
Atten, V. Pentu Alex, X. Phavare, P. D., Wilaket, R. George, S. Direction of umbilical Cord Twist
and characteristics 2013, (1) 1-4.
3.
Adesina, N. T., Ogunlaya, O. O., Aboyeji, P. A., Olaramoye, O. A., Adeniran, A.
S., Fakide, A. A. Umbilical cord parameter in Ilorin
correlate and Fetal Outcome, Eastern African Med. Journal 2014, 91 (8) 274-280.
4.
Valsamakis. G., Kanako, G., Malametisi Pirchner, A., Mostorajav, G.
cause of Intra-uterine growth restriction and post natal development of
metabolic syndrome. Ann. N. Y., Acad. Sci. 2006; (1092): 138-147
5.
Yelter, I. F.,
Examination of the placenta. Am Academy Fam. Physician 1998: 57; (5); 1045-1054
6.
Vanden Broek, N. Ntonya, C., Kayare, E., White, S., Nelson, J. preterm birth in rural
Malawi High Incidence in ultrasound dated population. Hum. Reprod.
2006, (20) 3235-3237
7.
Benischke, K. the
umbilical cord Neo-review 2009; 5(4) 34.
8.
Baergen, R. N., Maileaken, D., Brehlug, C., Benaschke, K. Morbidity, mortality and placenta morphology
in excessively long umbilical cord. Retrospective study pediatric Dev. Pathel 2001; 4(2) 144-153
9.
Maileaken, D., Brehlug, C., Benaschke, K.
Morbidity, mortality and placenta morphology in excessively long umbilical
cord. Retrospective study pediatric Dev. Pathel 2001;
4(2) 144-153
10.
Krakowale, P. Smit, E. N., de Brayn, G., Lydon Rochelli, M. T. Risk
factors and outcome associated with short umbilical cord. Obstet
Gynaecol 2004; 103 (I) 119-127
11.
Jason, A. Collins, Charles, L. Collins and Candance, C. Collins, perenata
umbilical cord project 2002, vol. 1
12.
Naeye, R. L.,
cause of perinatal mortality in the collaborative perinatal project 1977. 238;
228-229.
13.
Incerpi, M. H.,
Miller, D. A., Samadi, R., Settlage,
R. H., Godwin, T. M. stillbirth evaluation, what test are
needed. Am. J. Obstet Gynaecol
1998 178, 1121-25
14.
Alessandri, T. M.,
Stanley. F. S., Garner, J.B., Newnham, J., Walters,
BNJ, A case control study of unexplained ante-partum stillbirth Brit. J. Obstet Gynaecol 1992 99; 711-18
15.
Oron, T., Sheiner, E., Shoham Vardi, T., Mazor, M., Katz, M., Hallak, M., Risk factors for ante-partun
fetal death. J. Reprod. Med. 2001, 46; 825-30
16.
Kirukup, B.,
Welch, G., Normal but dead, perinatal mortality in non-malformed babies of
birth weight 2.5kg and over in the Northern region in 1983, Brit, J. Obtstet Gynaecol 1990, 97,
381-392
17.
Lee, K. S., Khoshmood,
B., Chen, I., Wall, S. N., Cromies, W. J. Mittendorf, R. L. infant mortality from congenital
malformation in the United States 1970-1997, Obstet Gynael 2001: 98, 620-627
18.
Namesi, A. K., Kohnen, G., Milovaov, A. P., Domogatsky, S. P., Kaifmain, P. strime Differentiation and architecture of the human
umbilical cord and placenta 1997; 18, 53-64
19.
Sarwono, E., Disse, W.S., Oudesluys Morphy, H. M., Oosting, H.,
Groot, C. J. umbilical cord length and intra uterine well
being 1991, 31, 136-40.
20.
Bernholtz, J. C., Eedose physiology of the fetus ultrasonography of supply
line deprivation syndromes Raduol Clin
North Aver 1990, 28, 179-88
21.
Amiel-Tison, C.,
Stewart, A. The newborn infant, one brain for life 1994, InSERM
Paris France
22.
Balkawade, N. U., Smude, M. A., study of umbilical cord and fetal outcome in
a study of 1000 deliveries obstetric gynaecol India
2012; (62), 520-525.
23
Malipa, P. Length of umbilical
cord at term, British Med. J. 1964 4(1) 674-4.
24.
Mishra, R., Jayalaxim,
P., Nirmala Kuren, J.
Correlation of the length of umbilical cord of the fetus with outcome in labour, J. Obstetric, Gyneacol,
India 1987, 37, 781
25.
Olaye, C. M. Immuno-histochemical protein expression profiting of growth
and apopotic related factors in relation to umbilical
cord length, early Hum Dev. 2015, 91(5) 2911-7.
26
Nilesh Unmesh Backawadi, Mangala Ashok Shinde. Study of
length of umbilical cord and fetal outcome. A study of 1000 deliveries. J. Obst. Gynaecol India 2012, 62(5)
520-525. Dec. 2007 – Oct. 2009
27
Yadav. B. B., Kordakar DVR, Darale, N. A.,
Correlation of umbilical cord length and fetal and maternal outcome. Journal of
evolution of medical and dental science 2013; 2 Issue (1-4)
28
Shunji Suzuki,
Yukiko Fuse. The length of the umbilical cord and perinatal outcomes in a
Japanese singleton pregnancies delivered at great than or equal to 34 weeks
gestation. Japans Med Journal 2012, Vol.1, 1-5
29
Birla Nandi, Jain Despal,
Bhatu Bilcapel, Are Shahken, Dhotre Jyathi Relationship between cord length and maternal and
fetal outcome. Pampex Indian Journal of Research
2015, Vol. 4, issue 7
30
Rayburn, W. F., Beynen,
A., Brinkman, D. L., umbilical cord length and intra-partum complication.
Obstet. Gynaecol 1981, 57; 450.
31
Anma, G., Kalante, E. Osmond, C. Erukson Koyal. A prospective, population based cohort study, Eur, previous, cordis 2015 22,
(9) 1154-60
32
Adinma, J. The
umbilical cord. A study of 1000 consecutive deliveries Int. Ferti
Menopausal study 1993-38 (3) 175-9
33
Agbola, A.
Correlation of human umbilical cord length Int. J. Gynaecol
Obstet 1979 16(3) 238-239
34
Ogunlaya, O. A., Ogunlaya, I.P. Correlation between umbilical cord length,
birth weight and birth length of singleton delivery at term in Nigeria
population 2015; (1) 1, 3
35
Naeye, R. L.
umbilical cord length and clinical significance Journal of Paediatric
1986, volume 157, issue 2, pg 278-280
36
Wright, D., Chas, G. M. fetal bone strength
and umbilical cord length Journal of Perinatology 2009, 29;, 603-605
37
Harold, F., Elston,
C. W. pathology of the umbilical cord, pathology of the placenta major
problems.
38
Spellency, M.,
Graven, H., Fischi, R. O. The umbilical cord
complication of true knot, Nuchal coils and cord around the body Am J., Obstet.
Gynaecol 1966, 94 (8) 1136-42
39
Donard, A., Des
Camp, P., Wigres, P., Mangante,
C., Gegore, J. A., Pourcalat,
D., Feorro, G., Lansar, J.,
Body, G., Pourcelot, C., in-utero measurement of the
umbilical cord in full term pregnancy. 1966 25(1) 78-86
40
La-Monica, Wilson, M.L., Fullulase,
A. M., minimal cord length that allows vaginal delivery. J. Reprod.
Med. 2008 53(3) 217-9
41
Olaya, M., Bernald, J. E. umbilical cord abnormalities in fetal and
neonatal pathology, in Biogote Achievers of perinatal
medicine. APM – 2014; (20) 22-27.
42
Jaykaran C and Tamoghna B. How to Calculate Sample Size for Different Styudy
Designs in Medical Research Indian
Journal of Psychol Med.2013, 35(2): 121- 126.
|
Cite this Article: Maduagwu AO; Okonkwo
C; Egwim VA; Ejelonu TU
(2021). The Relationship between Fetal Umbilical Cord Length And Fetal
Outcome. Greener Journal of Medical
Sciences, 11(1): 73-87.
|