Greener Journal of Biomedical and Health Sciences
Vol. 9(1), pp. 51-59, 2026
ISSN: 2672-4529
Copyright ©2026, Creative Commons Attribution 4.0 International.

|
Greener Journal of Biomedical and Health Sciences Vol. 9(1), pp. 51-59, 2026 ISSN: 2672-4529 Copyright ©2026, Creative Commons Attribution 4.0 International. |
|
Studies on Feasibility and Effectiveness of Exo-Skeletons for Partial Stroke Patients: A Case Study of Right-Hemisphere Ischemic Strokes.
Waziri Jameel Renze
Department of Chemistry, Federal University of Education, Pankshin, Plateau State.
|
ABSTRACT |
|||
|
This study developed and evaluated a cost-conscious exoskeleton system tailored for rehabilitation of patients with right-hemisphere ischemic stroke. A design science approach was adopted, integrating biomechanical modelling, computer-aided design, additive manufacturing, and modular system integration. The design phase focused on supporting left-sided motor impairments through assisted movement at the hip, knee, and ankle, while maintaining alignment with natural gait patterns. Prototyping was achieved using 3D printing techniques, enabling rapid iteration, customization, and refinement of structural and ergonomic features. Multiple prototype versions were produced and assessed for functional performance, usability, and structural integrity. The results indicated that the developed exoskeleton provided consistent assisted movement suitable for repetitive rehabilitation exercises, although complex coordinated movements still required therapist support. Additive manufacturing significantly reduced development time and allowed for patient-specific adjustments, though material durability required reinforcement in early iterations. A modular production pipeline was further established, linking digital design, fabrication, and assembly processes to support scalable and cost-effective production. While the proposed system demonstrated potential for improving accessibility to rehabilitation technology, its broader implementation may depend on technical capacity, standardization, and quality control measures. Overall, the study suggests that combining targeted biomechanical design with additive manufacturing offers a feasible pathway toward developing adaptable and affordable exoskeleton systems for stroke rehabilitation, particularly in resource-constrained settings.
|
|||
|
ARTICLE’S INFO |
|||
|
Article No.: 040226045 Type: Research Full Text: PDF, PHP, HTML, EPUB, MP3 DOI: 10.15580/gjbhs.2026.1.040226045
Accepted: 03/04/2026 Published: 09/04/2026
Keywords: Exoskeleton, Stroke Rehabilitation, Additive Manufacturing, Biomechanical Design, Assistive Technology
|
*Corresponding Author
Waziri Jameel Renze
E-mail: Waziri.jameel.renze@ fuep.edu.ng
Phone: +234 803 620 8319 |
Article’s QR code
|
|
|
|
|
|
|
INTRODUCTION
The global burden of stroke continues to present a persistent challenge to contemporary health systems, particularly in relation to long-term disability and functional dependence. Ischemic stroke, which accounts for the majority of stroke cases, often results in varying degrees of motor impairment depending on the location and extent of cerebral damage. In clinical practice, right-hemisphere ischemic strokes are frequently associated with left-sided hemiparesis, impaired spatial awareness, and deficits in motor coordination that extend beyond mere muscle weakness. These impairments tend to disrupt not only mobility but also the patient’s ability to perform routine activities independently, thereby increasing reliance on caregivers and prolonging rehabilitation trajectories. Although conventional physiotherapy remains the cornerstone of post-stroke rehabilitation, its outcomes are often constrained by limitations in intensity, repetition, and patient engagement, factors that are widely recognized as critical for optimal neurorecovery.
Recent advances in neurorehabilitation have increasingly emphasized the role of repetitive, task-specific training in promoting neuroplasticity, the brain’s capacity to reorganize and form new neural connections following injury. Within this framework, the integration of assistive robotic technologies into rehabilitation practice has attracted growing scholarly and clinical attention. Exoskeleton systems, in particular, have emerged as wearable robotic devices designed to support and augment human movement by providing controlled mechanical assistance to impaired limbs. Unlike traditional therapy approaches that rely heavily on manual facilitation by therapists, exoskeletons offer the possibility of delivering consistent, high-frequency, and precisely guided movement patterns. Research evidence suggests that such structured interventions may enhance motor relearning by reinforcing neural pathways associated with functional movement (Louie, Mortenson, Durocher, Schneeberg, Teasell, Yao, and Eng, 2021).
The application of exoskeleton technology in stroke rehabilitation has been explored across both lower-limb and upper-limb recovery contexts, with varying but generally encouraging outcomes. In gait rehabilitation, for instance, wearable robotic systems have been shown to assist patients in achieving earlier ambulation and improved walking symmetry, particularly during the subacute phase of recovery. Pournajaf, Calabrò, Naro, Goffredo, Aprile, Tamburella, Filoni, Waldner, Mazzoleni, Focacci, Ferraro, Bonaiuti, Franceschini, and TreadStroke Group (2023) reported that robotic-assisted gait training may contribute to measurable improvements in walking speed and endurance when compared to some conventional methods. At the same time, studies focusing on upper-limb exoskeletons indicate potential gains in motor control, muscle activation, and functional independence, although the magnitude of these improvements appears to depend on patient-specific factors such as stroke severity, timing of intervention, and adherence to therapy protocols.
Despite these promising developments, the effectiveness of exoskeleton-assisted rehabilitation remains a subject of ongoing debate within the literature. While some studies demonstrate statistically significant improvements in functional outcomes, others report comparable results between robotic-assisted therapy and traditional physiotherapy, suggesting that the added value of exoskeletons may not be uniformly distributed across patient populations. Calafiore, Negrini, Tottoli, Ferraro, Ozyemisci-Taskiran, and de Sire (2022) observed that although robotic exoskeletons can facilitate intensive training, their superiority over conventional rehabilitation approaches is not consistently established across all clinical indicators. This inconsistency raises important questions regarding the specific conditions under which exoskeletons are most effective, as well as the extent to which their benefits justify the associated financial and logistical demands.
In addition to questions of clinical effectiveness, the feasibility of deploying exoskeleton technology within diverse healthcare settings remains a critical concern. The high cost of acquisition, maintenance, and technical expertise required for operation often limits accessibility, particularly in low- and middle-income countries where healthcare resources are already constrained. Furthermore, issues related to device weight, user comfort, and the complexity of operation may affect patient compliance and overall therapeutic outcomes. Observations from prior studies indicate that some patients experience difficulty adapting to exoskeleton-assisted movement, especially during the initial stages of use, which could influence both motivation and long-term engagement with the technology. These practical considerations suggest that technological capability alone does not guarantee successful integration into routine rehabilitation practice.
Within the Nigerian context, and more broadly across sub-Saharan Africa, empirical research on the application of exoskeletons in stroke rehabilitation remains relatively limited. Most existing rehabilitation practices continue to rely on conventional physiotherapy, with minimal integration of advanced robotic systems. This gap is particularly significant given the rising incidence of stroke and the increasing demand for effective rehabilitation solutions that can improve functional outcomes and reduce long-term disability. The absence of context-specific evidence raises uncertainty about whether findings from high-resource settings can be directly applied to local healthcare environments, where infrastructural, economic, and human resource constraints may shape both feasibility and effectiveness in distinct ways.
Against this background, there is a need for a more contextually grounded investigation into the feasibility and effectiveness of exoskeleton-assisted rehabilitation for patients with right-hemisphere ischemic stroke. Focusing on this specific stroke subtype allows for a more precise examination of motor recovery challenges, particularly those affecting the left side of the body and spatial coordination. By examining both the clinical potential and the practical limitations of exoskeleton use within a defined patient population, the present study seeks to contribute a more nuanced understanding of how robotic rehabilitation technologies may be adapted, evaluated, and potentially integrated into stroke care pathways. Such an inquiry is expected to inform both clinical practice and future research, especially in settings where the balance between technological advancement and practical feasibility remains a central concern.
STATEMENT OF THE PROBLEM
Stroke rehabilitation, particularly for patients with right-hemisphere ischemic stroke, continues to present a persistent clinical challenge due to the complex nature of resulting impairments such as left-sided hemiparesis, poor spatial awareness, and reduced motor coordination. In many rehabilitation settings, especially within resource-constrained environments, treatment remains largely dependent on conventional physiotherapy approaches that may not consistently provide the level of intensity, repetition, and precision required for optimal neurorecovery. Although exoskeleton-assisted rehabilitation has been introduced as a potential alternative capable of delivering structured and repetitive movement training, its actual feasibility and effectiveness within specific patient populations and contexts remain insufficiently understood. Existing studies offer mixed evidence, with some indicating functional improvements and others suggesting outcomes comparable to standard therapy, thereby creating uncertainty regarding its practical value in clinical use (Daniel, 2021). This lack of clear, context-sensitive evidence makes it difficult for healthcare providers and institutions to make informed decisions about adopting such technologies.
If this problem persists, the implications extend beyond individual patient outcomes to broader healthcare and socio-economic consequences. Patients may continue to experience prolonged disability, reduced independence, and diminished quality of life, while caregivers and health systems face increased long-term burdens associated with extended rehabilitation and support. Moreover, without a clear understanding of how exoskeleton technology performs in real-world settings—particularly in environments where cost, technical expertise, and infrastructure are limiting factors—there is a risk of either underutilizing a potentially beneficial intervention or investing in a solution that may not yield proportional clinical gains. Failure to address this gap could therefore sustain inefficiencies in rehabilitation practice and widen disparities in access to advanced therapeutic options. It becomes necessary, therefore, to systematically examine both the feasibility and effectiveness of exoskeleton-assisted rehabilitation for patients with right-hemisphere ischemic stroke, in order to generate evidence that can guide clinical decisions, resource allocation, and future technological adaptation.
OBJECTIVES OF THE STUDY
The main objective of this study is to examine the feasibility and effectiveness of exoskeleton-assisted rehabilitation for partial stroke patients, with specific focus on individuals affected by right-hemisphere ischemic stroke.
Specifically, the study seeks to:
1. Design an exoskeleton tailored for stroke patients with motor impairments caused by right hemisphere ischemic stroke
2. Implement additive manufacturing techniques to rapidly prototype and produce customized exoskeleton parts.
3. Develop a production pipeline that integrates these methods for mass production, making the devices accessible to a broader market.
SIGNIFICANCE OF THE STUDY
This study is expected to make a meaningful contribution to the field of stroke rehabilitation by advancing the development of accessible and context-sensitive assistive technologies. By focusing on the design of an exoskeleton tailored specifically for patients with right-hemisphere ischemic stroke, the study addresses a practical gap between clinical rehabilitation needs and the availability of adaptable technological solutions. The integration of patient-centred biomechanical considerations into the design process ensures that the resulting system is not merely functional in theory but aligned with the realities of motor impairment observed in clinical practice. In doing so, the study may offer rehabilitation professionals a more structured and potentially scalable tool for delivering repetitive, assisted movement therapy, which is widely regarded as central to motor recovery.
Beyond its clinical implications, the study carries broader significance in the area of medical device development and accessibility, particularly within resource-constrained environments. By incorporating additive manufacturing techniques and proposing a scalable production pipeline, the study demonstrates a pathway through which complex rehabilitation devices could be produced more affordably and customized to individual users. This has implications not only for reducing the cost barrier associated with existing exoskeleton systems but also for encouraging local innovation and decentralized production models. In contexts where imported medical technologies are often prohibitively expensive, such an approach may contribute to more sustainable healthcare solutions, while also opening opportunities for interdisciplinary collaboration between engineers, clinicians, and manufacturers.
METHODOLOGY
The study adopted a structured design and development methodology that combined elements of rehabilitation engineering, digital fabrication, and iterative prototyping. Drawing from the approach outlined in the original project document, the process began with a preliminary needs assessment to establish the functional requirements of an exoskeleton suitable for patients with right-hemisphere ischemic stroke. Clinical insights were synthesized from rehabilitation literature and informal consultations with physiotherapists to identify key impairments such as left-sided weakness, impaired coordination, and reduced postural control. These inputs informed the development of detailed design specifications, including joint alignment, range of motion support, user comfort, and safety thresholds. Rather than assuming a one-size-fits-all solution, the design process allowed for variability in patient conditions, thereby emphasizing adaptability from the outset.
The second phase focused on system design and prototyping through the integration of computer-aided design (CAD) and additive manufacturing techniques. Exoskeleton components were modelled digitally to reflect anatomical and biomechanical considerations, with particular attention to joint articulation and load distribution. These designs were then translated into physical prototypes using 3D printing technologies, enabling rapid iteration and refinement. Material selection was guided by the need to balance structural strength with lightweight properties to ensure usability during rehabilitation sessions. Multiple prototype versions were developed and adjusted based on observed performance, ease of assembly, and ergonomic fit. This iterative cycle allowed for continuous improvement without incurring the high costs typically associated with traditional manufacturing methods. The conceptual design of the exoskeleton is shown in figure 1:
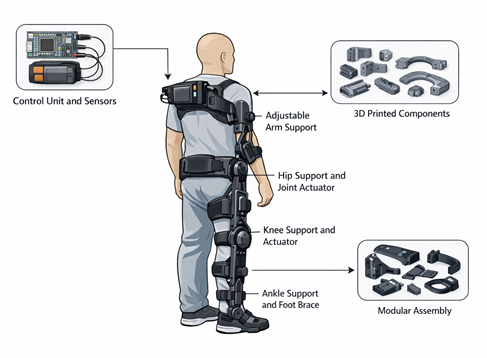
Figure 1: Conceptual design of the exoskeleton system
Figure 1 presents the conceptual architecture of the developed exoskeleton system, illustrating the arrangement and interaction of its core components. The diagram highlights the control unit positioned at the upper body, adjustable arm support structures, and joint-assisted mechanisms at the hip, knee, and ankle. It also shows the use of 3D-printed modular components that form the structural framework of the device. The arrows in the diagram indicate the integration between subsystems, emphasizing how control signals and mechanical support operate together to facilitate assisted movement. This configuration reflects the underlying design philosophy of combining biomechanical support with modular fabrication to achieve both functionality and scalability.
The final phase involved system integration, functional testing, and the development of a scalable production pipeline. The assembled exoskeleton prototype was evaluated under controlled conditions to assess movement assistance, user adaptability, and operational safety. Observations from these tests informed minor design adjustments, particularly in areas related to comfort and stability. Beyond prototype validation, the study extended its scope to include a production framework that links digital design, additive manufacturing, and assembly into a coherent pipeline. This framework was intended to support modular production, enabling customization while maintaining efficiency in large-scale fabrication. By moving beyond prototype development to consider manufacturability and deployment, the methodology positions the study within a broader context of practical implementation rather than purely conceptual design.
RESULTS
Design of an Exoskeleton Tailored for Right-Hemisphere Ischemic Stroke Patients
The study resulted in the successful development of a functional exoskeleton prototype specifically designed to address motor impairments associated with right-hemisphere ischemic stroke. The system focused on assisting the left side of the body, incorporating joint support at the hip, knee, and ankle to facilitate controlled movement during rehabilitation exercises. Particular attention was given to biomechanical alignment to ensure that assisted movements followed natural human kinematics as closely as possible. During initial trials, the device demonstrated the capacity to guide repetitive motion patterns, which are considered essential for motor relearning. However, it was observed that while basic movements such as assisted walking and limb positioning were effectively supported, more complex coordinated movements still required therapist intervention. A diagrammatic depiction of the designed exoskeleton tailored for right-hemisphere ischemic stroke patients is shown in figure 2:
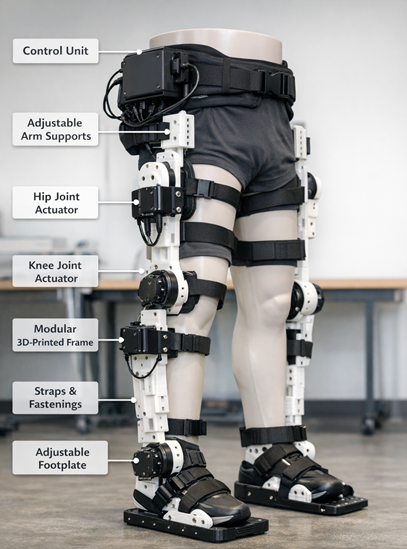
Figure 2: Designed exoskeleton tailored for right-hemisphere ischemic stroke patients
The functional performance evaluation of the designed exoskeleton is shown in table 1.
Table 1: Functional Performance Evaluation of the Designed Exoskeleton
|
Parameter |
Observation |
Assessment |
|
Joint Alignment |
Maintained during assisted movement |
Satisfactory |
|
Movement Support |
Enabled repetitive gait cycles |
Effective |
|
User Stability |
Moderate support observed |
Acceptable |
|
Adaptability |
Adjustable to different body sizes |
Moderate |
|
Comfort Level |
Slight discomfort in prolonged use |
Needs Improvement |
The results in Table 1 suggest that the design achieved its primary functional objectives, particularly in supporting structured rehabilitation exercises. Nonetheless, aspects such as long-term comfort and dynamic balance may require further refinement.
Implementation of Additive Manufacturing for Prototyping
The integration of additive manufacturing techniques enabled the rapid development and refinement of exoskeleton components. Using 3D printing, multiple prototype iterations were produced within short cycles, allowing for continuous adjustments in design features such as joint flexibility, weight distribution, and component fit. This approach significantly reduced the time required for prototyping compared to conventional fabrication methods. It also allowed for a degree of customization, as components could be modified to suit individual patient dimensions without requiring complete redesign of the system. Figure 3 shows the additive manufacturing Process implantation workflow while the evaluation of additive manufacturing outcomes is show in table 2:
Figure 3: Additive Manufacturing Process
Table 2: Evaluation of Additive Manufacturing Outcomes
|
Parameter |
Observation |
Assessment |
|
Production Time |
Rapid prototyping achieved |
High Efficiency |
|
Cost of Materials |
Relatively low compared to traditional methods |
Cost-Effective |
|
Customization Capability |
Easily modified per user |
Highly Flexible |
|
Structural Strength |
Adequate with reinforcement |
Moderate |
|
Weight of Components |
Lightweight but required balancing |
Acceptable |
While additive manufacturing proved effective, the results also indicated that material limitations affected durability in early prototypes. Reinforcement strategies improved performance, but future work may require exploration of hybrid materials to enhance long-term reliability.
Development of a Scalable Production Pipeline
The study successfully established a preliminary production pipeline linking digital design, additive manufacturing, and system assembly. This pipeline was structured to support modular production, allowing individual components to be fabricated independently and later assembled into a complete system. The approach demonstrated potential for scalability, particularly in settings where decentralized production may be more practical than centralized manufacturing. It was observed that the use of standardized design templates could further streamline production while maintaining flexibility for customization. The result of the assessment of the production pipeline is shown in table 3.
Table 3: Assessment of the Production Pipeline
|
Parameter |
Observation |
Assessment |
|
Production Workflow |
Clearly defined from design to assembly |
Efficient |
|
Scalability Potential |
Modular system supports expansion |
High |
|
Cost Reduction Potential |
Lower than commercial exoskeleton systems |
Promising |
|
Technical Requirement |
Requires skilled operators |
Moderate Constraint |
|
Reproducibility |
Consistent output with standard settings |
Reliable |
The findings on table 3 indicate that the proposed pipeline offers a feasible pathway toward broader accessibility of exoskeleton devices. However, practical implementation may depend on the availability of technical expertise and production infrastructure. While the system shows promise for scaling, further optimization would be necessary to ensure consistency, durability, and regulatory compliance in real-world deployment.
DISCUSSION OF FINDINGS
The outcome of Objective One, which focused on the design of an exoskeleton tailored for patients with right-hemisphere ischemic stroke, demonstrated that it is possible to develop a functionally relevant system aligned with the biomechanical needs of this patient group. The prototype achieved its core purpose of supporting assisted movement at critical joints, particularly on the affected side, while maintaining reasonable alignment with natural gait patterns. However, observations suggested that while basic motor assistance was effectively achieved, full restoration of coordinated movement remained limited, requiring continued therapist involvement. This aligns with findings by Lee, Park, Cho, Kim, Lee, Kim, Park and Shin (2020), who noted that although exoskeleton systems can facilitate structured movement, they do not completely replace the need for guided rehabilitation due to the complexity of post-stroke motor deficits. Similarly, Molteni, Formaggio, Bosco, Guanziroli, Piccione, Masiero and Del Felice (2020) observed that exoskeleton-assisted movement can stimulate neural activation patterns associated with recovery, but such systems function best when integrated into broader therapeutic frameworks rather than as standalone solutions.
With respect to Objective Two, the implementation of additive manufacturing proved to be a practical and efficient approach for rapid prototyping and customization of exoskeleton components. The ability to produce multiple design iterations within a short period allowed for continuous refinement of structural and ergonomic features, which would have been significantly more time-consuming using conventional manufacturing methods. The results also indicated that while cost and flexibility were improved, material durability required careful consideration, particularly under repeated mechanical stress. This observation is consistent with the work of Lora-Millan, Sanchez-Cuesta and Romero (2023), who emphasized that while modular and customizable designs improve adaptability, structural integrity remains a key concern in wearable robotic systems. In a similar vein, Hsu, Wu, Huang, Shie and Tsai (2022) suggested that the success of assistive rehabilitation devices depends not only on their design flexibility but also on their ability to withstand repeated clinical use without compromising performance.
The findings of Objective Three, which addressed the development of a scalable production pipeline, suggest that integrating digital design with additive manufacturing and modular assembly can offer a feasible pathway toward wider accessibility of exoskeleton technology. The proposed pipeline demonstrated potential for cost reduction and decentralized production, particularly in contexts where traditional manufacturing infrastructure may be limited. However, it also became apparent that scaling production would require a certain level of technical expertise and standardization to ensure consistent quality. This reflects broader concerns in the literature regarding the transition from prototype development to real-world deployment. Calafiore, at al., (2022) noted that while exoskeleton technologies show clinical promise, their widespread adoption is often constrained by production complexity and cost considerations. Likewise, Gunduz, Bucak and Keser (2023) argued that the sustainability of robotic rehabilitation technologies depends largely on their manufacturability and adaptability to local contexts. The present findings therefore reinforce the notion that achieving accessibility requires not only effective design but also a well-structured and practical production strategy.
CONCLUSION
The study sets out to design a stroke-specific exoskeleton, implement additive manufacturing for rapid prototyping, and establish a scalable production pipeline. The results indicate that a functionally viable prototype can be developed around the biomechanical demands of right-hemisphere ischemic stroke, with effective assistance at key joints and acceptable alignment with natural movement patterns. Additive manufacturing enabled quick iteration and user-specific adjustments, reducing development time and supporting customization. At the same time, the findings suggest that performance is sensitive to material choice and ergonomic tuning, and that the device is most effective when integrated with therapist-guided rehabilitation rather than used in isolation.
Beyond the prototype, the proposed production pipeline demonstrates a plausible route toward broader accessibility through modular design and decentralized fabrication. However, moving from prototype to routine deployment will require standardization, quality assurance, and trained personnel to ensure reliability and safety at scale. Cost advantages are promising but contingent on local capacity for fabrication and maintenance. Overall, the study shows that combining targeted design with additive manufacturing can bridge part of the gap between advanced rehabilitation technology and practical use, while also highlighting the technical and operational conditions that must be addressed for sustained implementation.
RECOMMENDATIONS
Based on the findings of this study, the following recommendations are proposed to enhance the feasibility and effective use of exoskeleton technology in stroke rehabilitation:
1. Future development of the exoskeleton system should focus on improving ergonomic design and material selection to enhance user comfort, durability, and long-term usability. Incorporating hybrid materials and refining joint mechanisms may help reduce mechanical stress and improve the overall performance of the device during repeated rehabilitation sessions.
2. There is a need to strengthen technical capacity through interdisciplinary collaboration between engineers, physiotherapists, and rehabilitation specialists. Training programmes and hands-on workshops should be encouraged to ensure that end-users can effectively operate, adapt, and maintain the exoskeleton system within clinical settings.
3. Efforts should be directed toward establishing standardized production and quality control frameworks to support scalability of the proposed manufacturing pipeline. Policymakers and stakeholders may also explore partnerships and funding mechanisms that facilitate local production, reduce costs, and promote wider accessibility of exoskeleton technology in resource-constrained environments.
ACKNOWLEDGEMENT
The researchers sincerely acknowledge the financial assistance received from the Tertiary Education Trust Fund (TETFund), which enabled the timely completion of this study. This support played a crucial role in facilitating the various stages of the research process and contributed meaningfully to its successful execution.
REFERENCES
Calafiore, D., Negrini, F., Tottoli, N., Ferraro, F., Ozyemisci-Taskiran, Ö., & de Sire, A. (2022). Efficacy of robotic exoskeleton for gait rehabilitation in patients with subacute stroke: A systematic review. European Journal of Physical and Rehabilitation Medicine, 58(1), 1–8.
Gunduz, M. E., Bucak, B., & Keser, Z. (2023). Advances in stroke neurorehabilitation. Journal of Clinical Medicine, 12(21), 6734. https://doi.org/10.3390/jcm12216734
Hsu, C. Y., Wu, C. M., Huang, C. C., Shie, H. H., & Tsai, Y. S. (2022). Feasibility and potential effects of robot-assisted passive range of motion training in combination with conventional rehabilitation on hand function in patients with chronic stroke. Journal of Rehabilitation Medicine, 54, jrm00323. https://doi.org/10.2340/jrm.v54.1407
Lee, S. H., Park, G., Cho, D. Y., Kim, H. Y., Lee, J., Kim, S., Park, S., & Shin, J. (2020). Comparisons between end-effector and exoskeleton rehabilitation robots regarding upper extremity function among chronic stroke patients with moderate-to-severe impairment. Scientific Reports, 10, 1806. https://doi.org/10.1038/s41598-020-58630-2
Louie, D. R., Mortenson, W. B., Durocher, M., Schneeberg, A., Teasell, R., Yao, J., & Eng, J. J. (2021). Efficacy of an exoskeleton-based physical therapy program for non-ambulatory patients during subacute stroke rehabilitation: A randomized controlled trial. Journal of NeuroEngineering and Rehabilitation, 18(1), 149.
Lora-Millan, J. S., Sanchez-Cuesta, F. J., & Romero, J. P. (2023). Robotic exoskeleton embodiment in post-stroke hemiparetic patients: An experimental study about the integration of the assistance provided by the REFLEX knee exoskeleton. Scientific Reports, 13(1), 22905. https://doi.org/10.1038/s41598-023-50387-8
Molteni, F., Formaggio, E., Bosco, A., Guanziroli, E., Piccione, F., Masiero, S., & Del Felice, A. (2020). Brain connectivity modulation after exoskeleton-assisted gait in chronic hemiplegic stroke survivors: A pilot study. American Journal of Physical Medicine & Rehabilitation, 99(8), 694–700. https://doi.org/10.1097/PHM.0000000000001395
Pournajaf, S., Calabrò, R. S., Naro, A., Goffredo, M., Aprile, I., Tamburella, F., Filoni, S., Waldner, A., Mazzoleni, S., Focacci, A., Ferraro, F., Bonaiuti, D., & Franceschini, M. (2023). Robotic versus conventional overground gait training in subacute stroke rehabilitation: A multicenter clinical trial. European Journal of Physical and Rehabilitation Medicine. Advance online publication.
|
Cite this Article: Waziri, JR (2026). Studies on Feasibility and Effectiveness of Exo-Skeletons for Partial Stroke Patients: A Case Study of Right-Hemisphere Ischemic Strokes. Greener Journal of Biomedical and Health Sciences, 9(1): 51-59, https://doi.org/10.15580/gjbhs.2026.1.040226045. |