By Ikegwuonu, NC; Nzotta,
CC; Anyanwu, CE; Okpaleke,
MS (2022).
|
Greener
Journal of Medical Sciences
Vol. 12(1),
pp. 145-150, 2022
ISSN:
2276-7797
Copyright
©2022, the copyright of this article is retained by the author(s)
https://gjournals.org/GJMS
|

|
Assessment of Ultrasound Quality Control Practices in
Anambra State, Southeast, Nigeria.
1Nwamaka C. Ikegwuonu, 2Christian
C. Nzotta, 2Chinedu E. Anyanwu
and 2Michael S. Okpaleke
1 Radiology Department,
Nnamdi Azikiwe
University Teaching Hospital, Nnewi, Anambra State, Nigeria.
2 Department of Radiography, Faculty of Health Sciences and Technology,
College of Medicine, Nnamdi Azikiwe
University, Nnewi Campus, Anambra
State, Nigeria.
|
ARTICLE INFO
|
ABSTRACT
|
|
Article No.: 042622042
Type: Research
Full Text: PDF, HTML, EPUB, PHP
|
Background: Ultrasound equipment quality
control (QC) checks ensure that faults are detected and corrected, to ensure
optimal equipment performance for good clinical outcome. Ultrasound
practitioners have an essential role in the QC of ultrasound
scanners. This study was aimed at assessing QC
tasks practiced by ultrasound practitioners in Anambra
state, Nigeria, and their compliance to recommended standards.
Materials and Methods: This
was a cross-sectional, questionnaire-based study carried out among 37
certified ultrasound practitioners. The hardcopy questionnaire made up of
questions on QC practices according to recommendations of the American
Association of Ultrasound in Medicine (AIUM) was used for data collection,
and included questions on: cleanliness, infection control and safety tasks,
and image display and performance tasks. The obtained data were analyzed
using descriptive statistics.
Results: The ultrasound practitioners showed good compliance
(86.1% - 100%) to infection control QC tasks of cleaning transducer, console and monitor of gel and
body fluid; good compliance to equipment physical/mechanical safety tasks
(61.1% - 83.3%), but poor compliance to image display and performance tasks
(0 – 30.6%). Their compliance to the recommended frequency of practice for
these QC tasks was generally poor (0% - 19.4%), except for transducer
cleaning after each patient (91.7%) and immediate cleaning of spilled body
fluid (100%). All phantom tasks had zero practice among the practitioners. Though none of the facilities had a QC programme in place, in addition to poor awareness (33.3%,
n= 12)) of recommended QC tests by the practitioners, most (94.4 %, n=34) of
the practitioners believed that ultrasound quality control was beneficial.
Conclusion: Except for the phantom-based
tasks which had zero practice, other quality control tasks were practiced by
the ultrasound practitioners, and in varying degrees, but most times not
according to the recommended standards.
|
|
Accepted: 26/04/2022
Published: 30/04/2022
|
|
*Corresponding Author
Nwamaka
C. Ikegwuonu
E-mail: ncikegwuonu@ nauthnnewi.org.ng, zubeamaka@
yahoo.com
Phone: +2348033950499
|
|
Keywords: Ultrasound,
Quality control, Image quality.
|
|
|
|
Abbreviations: (IPEM) Institute of physics and engineering
in medicine; (RCR) Royal College of Radiologists; (ACR) American College of
Radiology; (AAPM) The American Association of Physics in Medicine; (EFSUMB);
European Federation of Societies for Ultrasound in Medicine and Biology.
INTRODUCTION
Ultrasound
equipment undergoes deterioration as a result of usage and normal aging
process.
Its delicate parts can be physically damaged by improper use and handling [1].
Transducers may be accidentally dropped, wheels may be run over cables, dust or
fluid may accumulate on the machine and its electrical boards, connecting ports
may become loose, cracks may appear on the knobs due to pressure of touch etc.
These factors collectively affect the imaging performance of an ultrasound
system. Some changes in performance may be obvious and usually noticed by the
operator; however, others may occur subtly over time and usually go unnoticed,
while some other problems may go unnoticed because they are masked by patient
anatomy [2]. Regular quality control checks are essential in detecting fault
that may affect equipment performance. Ultrasound QC is aimed at ensuring
proper equipment functionality, clinical usage safety within internationally
accepted limit, and performance consistency over time [3]. Ultrasound quality
assurance (QA) guidelines and recommendations have been developed by regulatory
bodies like AIUM, IPEM, RCR, ACR, AAPM, EFSUMB which if applied, will help in
maintaining high equipment performance for better diagnostic accuracy. A substantial effort has been made to determine the most
pertinent tests, the recommended frequency of testing, the most useful phantom
design(s) and acceptable measured values [2]. Some QA procedures are those that
are routinely carried out under good clinical practice, and consist of regular
safety and cleanliness checks as well as more detailed checks of image display
and performance which are best done using a phantom or a test object [4].
Ultrasound practitioners
have an essential role in the QA of ultrasound scanners [5]. A
clean and hygienic equipment including transducers, control panel, monitor,
and peripherals is mandatory each time before a patient is scanned [3]. In addition, adopting infection control
procedures ensures that the risk
of infection to patient and staff are minimized [5]. Visual inspection of
scanner’s physical components ensures that damaged components that may pose
electrical safety risks are identified and replaced. QC tests using phantom or test object
can provide insight to specific performance characteristics of an ultrasound
scanner [2]. The operator of the
ultrasound equipment should monitor its optimal operation and
immediately report any deficiency or fault for repairs [1].
Some studies in Nigeria have shown
poor quality control practices among ultrasound practitioners [6,7]. This study was therefore aimed at assessing
the quality control practices carried out by ultrasound practitioners in Anambra state, Nigeria.
MATERIALS AND METHODS
This was a descriptive
cross-sectional study carried out among 37 certified ultrasound practitioners practicing
in the 25 ultrasound facilities in
Onitsha, Awka, and Nnewi, Anambra State. An ethical approval
(NAUTH/CS/66/VOL.11/035/2018/031) for this study was obtained from the Human
Research and Ethical Committee of the Nnamdi Azikiwe University Teaching Hospital, Nnewi,
Anambra State, Nigeria. The
entire procedure of the study was adequately explained to the participants and
their consent was duly sought and obtained. All the information obtained was
treated with confidentiality and used for the purpose of this study only. A questionnaire was used to obtain information from the
participants. The questionnaire was validated using content validity, while its
reliability was tested using test-retest method; the cronbach’s
alpha reliability coefficient being 0.804. The questions were about electrical
safety, cleanliness and infection control, image display and performance,
according to AIUM recommendations. Questions to determine the priority given to
ultrasound QA were also included and bothered around the availability of formal
QA in place, awareness of ultrasound QC, frequency of QC actions and
availability of tissue-equivalent phantom. Opinion on the usefulness of
ultrasound QC was equally sought. A total of 37 Questionnaires were
self-distributed to the ultrasound practitioners working in the selected
centers. Thirty-six (36) were
filled by the respondents and collected back by the researcher, giving a 97%
return rate. Data were analyzed using a statistical package for social sciences
SPSS version 22. Non-numeric performance parameters and quality control
practices by ultrasound practitioners were expressed using simple descriptive
statistics (mean, frequency and percentages).
RESULTS
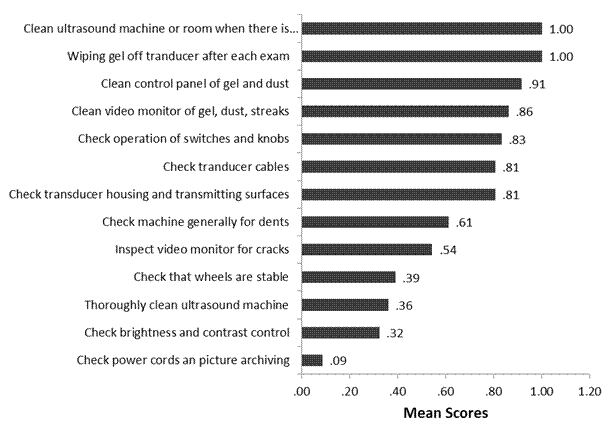
The results of the ultrasound
practitioners’ quality control practices revealed that the tasks of cleaning of
ultrasound machine or room, and wiping gel off transducer after each exam had
the highest mean score of 1.00 each respectively, while checking power cords
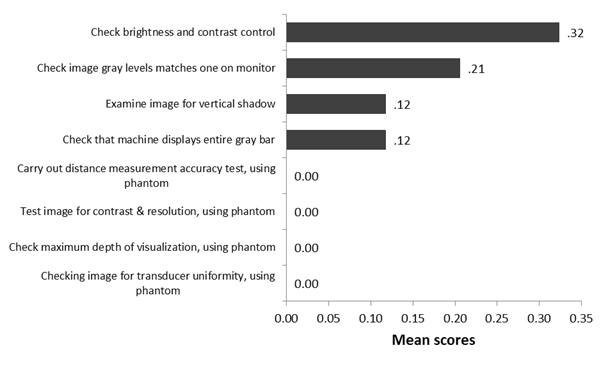
and picture archiving had the least mean score 0.09 (Figure 1). Tasks involving
use of phantom had zero score (figure 2)
DISCUSSION
Results
from our study showed that none of the facilities had a formal QA program in
place. This finding is consistent with the report of BMUS [8], which stated
that many clinical ultrasound services have no formal QA program. We therefore
infer that quality assurance is not prioritized in these facilities. In
addition, there is poor awareness among the ultrasound practitioners about the
quality control tests to be carried out on the ultrasound equipment,
nevertheless, most of the practitioners acknowledged the benefits of ultrasound
quality control.
In our
study, quality control tasks of equipment cleanliness, infection control, and
safety have good practice compliance by most of the practitioners, but their
compliance to the recommended frequency of practice was generally poor, except
for the cleaning transducer of gel after each patient, and cleaning spilled
fluid, both which has excellent compliance. Also, except for the scanners’
monitor which had good dust-cleaning practice compliance by the practitioners;
other tasks of cleaning equipment of dust have poor practice compliance among
the practitioners. Tasks for image display and performance by the ultrasound
practitioners were found to be poorly practiced, while their adherence to the
frequency of practice was even poorer. We found that all phantom-based tasks
had zero compliance, likely due to absence of QC phantom in all the facilities.
Our findings of poor compliance to some QC practices and poor compliance to
their recommended frequency of practice may not be unconnected with poor
awareness of QC tests noted among the ultrasound practitioners. However,
despite the poor awareness of QC tests, some of the practitioners showed
excellent compliance to some of the recommended QC practices, likely as a
result of good clinical practice, infection control consciousness and equipment
care. The is in agreement with the AIUM [4], which stated that some QA
procedures were those that are routinely carried out as good clinical
ultrasound practice, and the BMUS [8], which noted that some elements of QA
were not time-consuming and would already be carried out in departments
complying with local infection control and equipment management requirements.
Poor compliance to some QC tasks in this work may also be because of the lack
of a formal QA program in the facilities, which may lead to a lack of commitment
to QC.
Phantoms
are used to carry out measurable parameters in the ultrasound scanner and help
to reveal system defects that may otherwise not be identified and which can
affect patients’ diagnoses. However, QC phantoms are usually expensive and this
may have discouraged their procurement by the facilities we studied, and thus
zero compliance to all phantom-based tests. In addition, evidence of a current
QA certification is not required for setting up and continuing an ultrasound
practice in Nigeria, so the facilities may not readily commit funds for
something that has no legal threats. This agrees with Ward and Stanton [9] who
noted that time and resources may not be prioritized to something that is not
legally required. The ultrasound operators however believed that ultrasound QC
was beneficial. A good practice of quality control in ultrasound is beneficial
for improved clinical outcomes.
CONCLUSION
This study
revealed that ultrasound practitioners in Anambra
state undertake the various recommended ultrasound quality control tasks in
varying degrees but not according to recommended frequency of practice. QC
tasks involving the use of phantom was entirely lacking among the
practitioners. This may result in use of equipment with possible compromised
performance, which may affect clinical outcome.
Conflict
of interest: None was declared among the authors.
Funding
sources: None
Acknowledgment:
Not
applicable
REFERENCES
1)
Grazhdani, H., David, E., Spagnolo,
V.O., Buemi, F., Perri, A.,
Orsogna, N., Gigli, S, Chimenz, R . Quality assurance of
ultrasound systems: current status and review of literature. Journal of Ultrasound, 2018; 27(3), 173-182.
2)
Kofler, J.M. Quality assurance of ultrasound imagers:
Procedures, expectations and philosophies. The American Association of
Physics in Medicine (AAPM), 43rd Annual Meeting, 2001, P.5.;
Retrieved from: https://www.aapm.org/meetings/2001AM/pdf/7194-74902.pdf.
(Accessed on: 22/07/17).
3)
Kollmann, C., deKorte, C., Dudley, N.J., Gritzmann,
K. and Evans, D.H. (2012). Guidelines for technical quality assurance (TQA) of utrasound devices (B-Mode)-version 1.0. EFSUMB Technical
quality assurance group.US-TQA/B. Ultraschall
in Medicine, 33, 544-549.
4)
American Institute of Ultrasound in Medicine.
(2008). Routine quality assurance for
diagnostic ultrasound equipment. American Institute of Ultrasound in
Medicine, AIUM, Routine Quality Assurance of Clinical Ultrasound Equipment
Subcommittee. USA: Laurel MD.
5)
Dudley, N., Russell, S., Ward, B. and
Hoskins, P. (2014). British Medical Ultrasound Society guidelines for the
regular quality assurance testing of ultrasound scanners by sonographers: BMUS
Working Party. Ultrasound, 22(1),
8-14.
6)
Eze, C.U., Eze, C.U, Asogwa, C. A survey of
quality of sonographic practice. British Journal of Healthcare Management, 19(3), 2013:124-128.
7)
Sidi, M., Sani, G.M., Ya’u,
A., Zira, J.D, Loshugno, S.S, Luntsi, G. The current status of
ultrasound practice in Kano metropolis, Nigeria. Egyptian Journal of
Radiology Nuclear Medicine. 2021; 52, 212.
https://doi.org/10.1186/s43055-021-00509-x (Accessed on 13/9/21).
8)
British Medical Ultrasound Society. (2015). Guidelines for professional ultrasound
practice. Society and College of Radiographers and British Medical
Ultrasound Society. P. 9. Retrieved from: https://www.bmus.org/static/uploads/resources/SCoR__BMUS__Guidelines_Amend_Mar_2019_final_DecHwyx.pdf.
(Accessed on: 25/08/17).
9)
Ward, A.M, Stanton, M.T. Quality assurance in
Irish ultrasound departments. Poster
presentation (poster No:B-0715) to the European
Society of Radiology.2016. Retrieved from:
https://doi.org/10.1016/B978-0-08-102216-0.00003-5.
(Accessed on: 22/03/2017)