By Nwachukwu, C; Azuoma KE; Ugwunze,
AU; Enwelum, HO; Nwozor, CM
(2022).
|
Greener
Journal of Medical Sciences
Vol. 12(2),
pp. 178-184, 2022
ISSN:
2276-7797
Copyright
©2022, the copyright of this article is retained by the author(s)
https://gjournals.org/GJMS
|

|
Assessment of
Knowledge of HIV and its Impact on the Sexual Behaviour
of Chukwuemeka Odumegwu Ojukwu University (COOU) Students, Igbariam
Campus.
1Nwachukwu C., 1Azuoma K.E., 1Ugwunze A.U.,
1Enwelum H.O., *2Nwozor C.M.
1
Department of Community Medicine, Chukwuemeka Odumegwu Ojukwu University, Awka Campus. Anambra State.
Nigeria
2
Department of Physiology, Faculty of Basic Medical Sciences, Chukwuemeka Odumegwu Ojukwu University, Uli Campus.Anambra State. Nigeria.
|
ARTICLE INFO
|
ABSTRACT
|
|
Article No.: 111322093
Type: Research
Full Text: PDF,
HTML,
PHP,
EPUB
|
Human Immunodeficiency Virus (HIV) targets the body’s immune system
making it weak to fight infections and some kinds of cancers that would have
been fought in normal immune condition. Without treatment, it has a tendency
of progressing to acquired immunodeficiency syndrome (AIDS).This study was
undertaken to ascertain the knowledge of HIV, as well as its medical
management and its impact on sexual behaviour
amongst undergraduates of Chukwuemeka Odumegwu Ojukwu University
(COOU) Igbariam campus. Multistage sampling method
was used. Semi-structured self-administered questionnaires were distributed
to two hundred and seventeen (217) Arts students of Chukewuemeka
Odumegwu Ojukwu
University Igbariam campus. The results showed
that 209 (96.3%) students responded. Variable numbers of the respondents
were mainly from the departments of Economics (10%), Education (1.4%), Law
(41.6%), Political Science (25.4%), Psychology (17.2%) and Arts and Social
Science (4.3%).The older age group (≥25 years) and the married/co-habiting/others
were more knowledgeable of HIV than the younger respondents and the single,
respectively. The differences were statistically significant, (P=0.028).
However, males were significantly more knowledgeable than females (P=0.001).
Also, those that did not reveal whether they had ever had sex or not, as
well as those who had never had sex were more knowledgeable than those who
had ever had sex (P = 0.002). This was also statistically significant. In
conclusion, significantly increased number of the respondents had very good
knowledge of HIV, its management and prevention. However, only 30.1%
actually used condom. Also the results showed that HIV was well known even
among the non-medical students.
|
|
Received: 13/11/2022
Accepted: 23/11/2022
Published: 09/12/2022
|
|
*Corresponding Author
Nwozor, C.M.
E-mail: corneliusnwozor @gmail.com
|
|
Keywords: HIV/AIDS
knowledge, HIV/AIDS treatment, sexual behaviour,
undergraduate students
|
|
|
|
INTRODUCTION
Human
Immunodeficiency Virus (HIV) targets the body’s immune system making it
weak to fight infections and some kinds of cancers. Without treatment it can
progress to acquired immunodeficiency syndrome (AIDS). AIDS is caused by human
immunodeficiency virus types 1 and 2 (Bhatti et al., 2016). AIDS was first
recognized as a new disease in the year 1981. It was increasingly noticed
amongst homosexual men who usually had opportunistic infections and rare
malignancies (Sharp and Hahn 2011).
HIV
does not thrive in vitro. Mode of
transmission of the virus is via direct exposure to infected blood or
secretions in the presence of skin damage by needles or blades, abrasions in
mucosal tissues during sexual intercourse, from mother to child (Suligoi et al., 2010).
According
to UNAIDS, 38.4 million people worldwide were infected with HIV in 2021. 1.5
million people became newly infected with HIV in the
same year. 650, 000 people died from AIDS-related illnesses, while 40.1 million
people have died from AIDS-related illnesses since the beginning of the
pandemic. In 2021, the estimated number of HIV-positive people accessing
antiretroviral therapy was 28.7 million (UNAIDS, 2022).
In
2019, prevalence of HIV in Nigeria was 1.4% among those within the age range
15-19 years. Previous estimates had indicated a national prevalence of 2.8%.
UNAIDS and the National Agency for the Control of AIDS estimated that there
were 1.9 million people living with HIV in Nigeria (UNAIDS, 2022).
Sexuality
can be said to be intimately associated with physical and mental health, which
triggers thoughts, feelings, expressions, as well as interactions that are
related to sex, intimacy, and reproduction (Van der Slui
et al., 2016). Research on sexual behaviours and/or
expressions has shown that risky sexual behaviours (unprotected vaginal, oral or
anal intercourse) predispose to sexually transmitted infections (STIs). Young
students that commence sexual intercourse early in life are at a greater risk
of getting pregnant or contracting an STI than those who chose to postpone
their initiation time for sexual activities (Glen-Spyron,
2015). The impacts of these risky behaviours are manifested in the economic and
psychosocial costs, in addition to sexually transmitted infections (Tu et al., 2018; Waktole, 2019).
METHODOLOGY
Study Design
It was a
descriptive, cross sectional study using semi structured questionnaires which
were distributed to students of Chukwuemeka Odumegwu Ojukwu University, Igbariam campus between May and June 2022. Questionnaire was
pretested among 20 students for completeness, correctness and necessary
modification. Questionnaire used as pre-test was not included in the main
study.
Inclusion
Criteria: non Science students of COOU who were believed to have no strong
knowledge of HIV, first, second, third, fourth year students.
Exclusion
Criteria: students who were unwilling
to participate, students who were not available at the time of Study.
Study
Population
The study
population included the students of the Faculty of Arts, Chukwuemeka
Odumegwu Ojukwu University,
Igbariam campus
Sample Size
Determination: Using
} n = z²pq/ d²
Where
n = desired sample size (when population is greater
than 10,000.
z= standard normal
deviate usually set at 1.96 which corresponds to the 95% confidence level.
p= proportion of the target population
estimated to have a particular characteristics. If none use 50% (0.50).
q = 1.0 –p = 1- 0.5 = 0.5
d = degree of accuracy desired
usually set at 0.05 or 0.02 (Pourhoseingholi et al.,
2013)
Data
Collection Methods
The validity and credibility of the
questionnaire was ascertained by subjection to a mini survey before being used
for data collection from participants using a standardized, self-administered
questionnaire.
For sake of compliance, questionnaires were
administered to the students after their lectures during free periods and
attempts were made to collect them the same day.
Data Management
Plan
·
Knowledge of HIV
was assessed using the following parameters: mode of transmission, population
at risk, and mother-to-child mode of transmission. Ten questions were
used to assess respondent’s knowledge of HIV.
·
Each correct knowledge question was scored 2
and each wrong knowledge question had a score of 1. Total score was computed
for each respondent. Knowledge scores 10-14 and 15-20 were considered poor and
good knowledge, respectively.
·
Free medical
services were assessed using knowledge of drug treatment of HIV and centre were
free antiretroviral drugs can be obtained
·
Impact on sexual
behaviour was assessed using: abstinence, sexual practices and protective
measures taken during, before and after sexual activity.
Data Analysis
The data
collected were analysed using Statistical Package for Social Science (SPSS)
version 21. Data analysis included appropriate tables of frequencies,
percentages, proportions, mean, and diagram of relevant variable (bar charts,
pie charts)
Ethical
Consideration
Ethical
clearance was obtained from Chukwuemeka Odumegwu Ojukwu Igbariam Campus. The aim of this study was explained to the
participants and informed consent (verbal and written) was obtained before
administering each questionnaire. Participants’ confidentiality was ensured by
excluding names in the questionnaire.
RESULTS
Socio-
Demographic
A total of 217 questionnaires were
administered randomly to non-science students of Chukwuemeka
Odumegwu Ojukwu University,
Igbariam Campus. Only 209 students responded, giving
a response rate of 96.3%. A total of 9 (4.3%) students responded from the Department
of Art and Social Science Education, 21 (10%) respondents from the Department
of Economics, 3 (1.4%) respondents from the Department of Education Science, 87
(41.6%) respondents from the Department of law, 53 (25.4%) respondents from the
Department of Political Science, and 36 (17.2%) respondents from the Department
of Psychology.
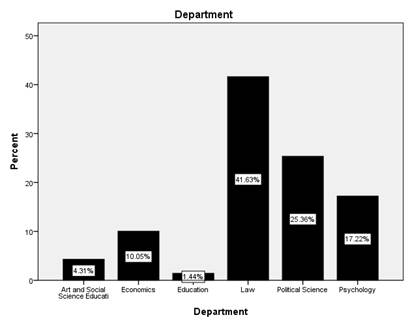
Fig. 1: Percentage
Distribution of Department
59 (28.2%)
of the respondents were between the age of 17- 19 years (Group 1), 144 (68.9%)
of the respondents were between the age of 20- 26 years (Group 2), 6 (2.8%) of
the respondents were between the age of 39- 55 years (Group 3).
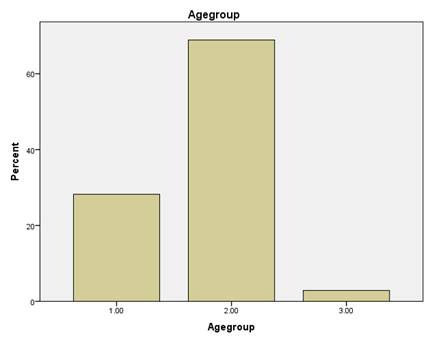
Fig. 2: Age
Distribution
Out of the 209 sample population, 82 (39.2%)
of the respondents were males and 127 (60.8%) were females.
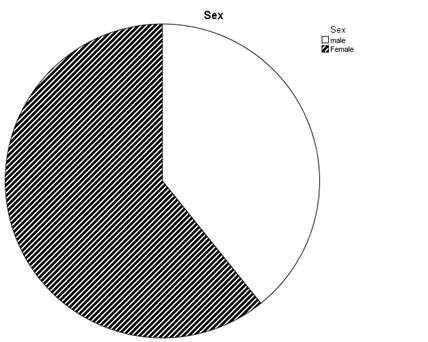
Fig. 3:
Sex Distribution
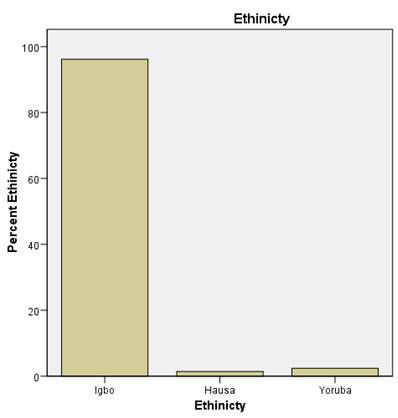
Fig.
4: Ethnicity
201 of the respondents were Igbo (96.2%), 3
(1.4%) were Hausa, and 5 (2.4%) were Yoruba.
200 (95.7%) of the total sample population
were single, 3 (1.4%) were married and 6 (2.9%) were separated. 206 (98.6%) of
the total sample population were Christians while 3 (1.4%) were traditional
worshippers.
Knowledge
of HIV
Ten questions were used to assess
respondent’s knowledge of HIV. 123 (58.9%) respondents said that HIV could be
spread through saliva and 76 (36.4%) respondents answered no, while 10 (4.8%)
respondents did not give any answer.203 (97.1%) respondents agreed that Needle prick injury from a used needle could transmit HIV virus and 4 (1.9%) respondents
answered no, while 2 (1.0%) respondents did not give any answer.206 (98.6%)
respondents said that multiple
sexual partners could increase the risk of HIV infection and 3 (1.4%)
respondents answered no.
183 (87.6%) respondents said that HIV could be transmitted from mother to child through breastfeeding
and
24(11.5%) respondents answered no, while 2 (1.0%) respondents did not give any
answer.29(13.9%) respondents agreed that long distance drivers were more predisposed to HIV Infection and 142
(67.9%) respondents answered no, while 38 (18.2%) respondents did not respond
to the question.195 (93.3%) respondents agreed that sex workers were predisposed to HIV infection and 11(5.3%)
respondents answered no, while 3 (1.4%) respondents did not respond to the
question.207 (99.0%) respondents agreed that HIV Infection could be contracted through blood transfusion and 2 (1.0%) respondents
answered no.
18 (8.9%) respondents agreed that HIV/AIDS could be treated completely and 186 (89.0%)
respondents answered no, while 5 (2.4%) respondents did not respond to the
question.159 (76.1%) respondents agreed that HIV infected person could be very healthy and 41 (19.6%) respondents answered no,
while 9 (4.3%) respondents did not respond to the question.
Sexual
Behavior
A good number 80
(38.3%) of the respondents admitted to having had sex before, while majority of
them 82 (39.2%) indulged in male-female kind. In the past 12 months majority 79
(37.8%) didn’t know the number of partners they had sex with while many 63
(30.1%) stated that they had with only one. Most of the respondents 63 (30.1%)
admitted to having used condom the last time they had sex. However on the issue
of prevention most of the respondents 122 (58.4%)
opted for abstinence as the most reliable method of prevention. Many opted for
vaginal sex as the kind of sex to be avoided as a way to reduce HIV infection
as against oral, anal sex and sex toys. Before having intercourse with a
new partner majority of the respondents170 (81.3%) agreed that one should
confirm the HIV status of himself/herself.
Table below shows the association between some of the
respondent’s characteristics and knowledge of HIV. The older age group
(≥25 years) and the married/co-habiting/others were more knowledgeable of
HIV than the younger respondents and the single, respectively. But the
differences were not statistically significant (p = 0.387).
However, males were significantly more
knowledgeable than females (p <0.001). Also, those that did not reveal
whether they had ever had sex or not, as well as those who had never had sex
were more knowledgeable than those who had ever had sex, p = 0.002. This was
also statistically significant.
Table: Respondents’ characteristics and
knowledge of HIV
|
Characteristics
|
Knowledge
|
|
|
Good
n (%)
|
Poor
n (%)
|
χ2
|
p-value
|
|
Age
≤ 24
≥25
|
124 (63.6)
11 (78.6)
|
71 (36.4)
3 (21.4)
|
Fisher’s exact
|
0.387
|
|
Sex
Male
Female
|
65 (79.3)
70 (55.1)
|
17 (20.7)
57 (44.9)
|
12.707
|
<0.001*
|
|
Marital
status
Single
Married/others
|
126 (63.0)
9 (100.0)
|
74 (37.0)
0 (0.0)
|
Fisher’s exact
|
0.028*
|
|
Ever had
sex
Yes
No
Rather not say
|
43 (53.8)
50 (63.3)
40 (83.3)
|
37 (46.3)
29 (36.7)
8 (16.7)
|
11.482
|
0.002*
|
*Statistically significant
DISCUSSION
The study assessed
the level of knowledge, management of HIV and its impact on sexual behaviour of undergraduate
students. The study showed that some of the students were knowledgeable of HIV,
including its aetiology, mode of transmission, and drug treatment. This we
believe may aid in the diminishing of the number of transmission of the
infection from one person to another as well as reduce the number of those
living with HIV. Our findings agree with that of Srivastava et al., (2021) who
reported that awareness of HIV was more in the adolescent age group.
The results of this study carried out
on COOU Igbariam students showed that majority of the
students despite being of non-medical discipline were significantly aware of
HIV. This is similar to knowledge of HIV result of the study carried out by Unadike et al., (2012) amongst preclinical students of
university of Uyo on awareness, knowledge and
perception of HIV/ AIDS and sexual behaviour. The difference was in condom use.
Their study showed that about 83.9% could identify the routes of transmission,
with 70% condom use. In our study we recorded condom use of 30.1%. Low condom
use may lead to high incidence of STIs and unwanted pregnancy. In matters of
HIV/ AIDS prevention is better than cure. Condom use is preventive. More
attention needs to be paid to this aspect of prevention.
The prevalence of HIV is a worldwide
threat to public health. There is still no cure for HIV. In addition to drug
treatment that prolongs the lives of those infected, health education is one of
the most effective preventive measures (Dokubo et
al., 2014).
On the aspect of sexual behaviour,
from the finding of this study only 30.1% actually used condom regularly during
sexual intercourse despite their knowledge of condom as being protective
against HIV infection. This is similar to the study carried by Izekor et al (2014). They reported low practice of condom usage
among sexually active students in a tertiary institution. The use of condom is
one of the best methods of coital practices that would protect one from contracting
the disease. Low condom use has strong implication for HIV transmission,
including STIs.
When asked however, about the number
of partners they have had intercourse with in the past one year, about 30% of
the study group stated one partner. 37.8% did not know the number of partners
they had sex with.
On the aspect of the effect of
knowledge of HIV on the sexual behaviours of COOU Igbariam
non-medical students one may say that knowledge of HIV may influence the sexual
behavioural practices of the tertiary students positively as many of the
respondents responded correctly on the questions posed to denote their level of
acquaintance on safe sexual practices. The study revealed that if one was
knowledgeable enough about HIV it extended also to one’s awareness of some
facts about medical management of HIV for those infected and for those trying
to prevent it on account of exposure. Our findings revealed that despite high
knowledge of HIV the use of condom, one of the key aspects of prevention, was
low. This agreed with that reported by Ugwu et al.,
(2022). They documented a contraceptive use of 34.6% despite increased
awareness of HIV. Up to 90% said that use of ART can significantly reduce the
burden of the ailment as well as help in improving the lives of the already
infected individuals.
CONCLUSION
In conclusion HIV awareness, drug treatment,
and its impact on the sexual behaviours among the study group of non-medical students
could be said to be high. However condom
use was low. In addition, being aware of HIV influences positively the sexual behaviour,
willingness to be tested, access to antiretroviral drugs, and other medical
services offered to HIV/AIDS patients.
REFERENCES
Bhatti AB, Usman M., Kandi V (2016). Current Scenario of HIV/AIDS, Treatment
Options, and Major Challenges with Compliance to Antiretroviral Therapy. Cureus. 8(3): e515. DOI 10.7759/cureus.515.
Dokubo, EK, Shiraishi RW, Young PW, Neal, JJ, Aberle-Grasse,
J., Honwana, N., Mbofana,
.F (2014). Awareness of HIV Status, Prevention Knowledge and Condom Use among
People Living with HIV in Mozambique.. PLoS ONE 9(9): e106760. doi:10.1371/journal.pone.0106760.
Glen-Spyron C (2015). Risky
Sexual Behavior in Adolescence. Belia
Vida Centre, Namibia.
Izekor S, Osifo U, Orhue P, Momoh A, Airhomwanbo K (2014).
Knowledge and practice of condom-usage among undergraduate students in Edo
State, Nigeria. IJCR, 3: 12-18.
Izekor S, Osifo UC, Orhue PO, Momoh A.R.M and Airhomwanbo KO
(2014). Knowledge and practice of condone- Usage among undergraduate students
in Edo State University. International Journal of Community Research. 3(1): 12-
18.
Pourhoseingholi MA,
Vahedi M, and Rahimzadeh M
(2013). Sample size calculation in medical studies. Gastroenterol
Hepatol Bed Bench 6(1): 14-17.
Sharp PM and Hahn BH
(2011). Origins of HIV and AIDS Pandemic. Cold spring Harb Perspect Med 1:a006841.
Srivastava S, Chauhan
S, Patel R. and Kumar P (2021). A study of awareness on HIV/ AIDS among
adolescent: a longitudinal study on UDAYA data. Scientific reports. 11:22841. https://doi.org/10.1038/s41598-021-02090-9.
Suligoi B, Raimondo M, Fanales-Belasio E, Buttò S (2010). The epidemic of HIV infection and AIDS,
promotion of testing, and innovative strategies. Ann Ist Super Sanità. ;
46:15-23.
Tu M., Saraiva G. and Id F (2018). Factors associated with family,
school and behavioural characteristics on sexual initiation: a gender analysis
for Brazilian adolescents. PLoS One, 13(12):
e0208542, doi: 10.1371/journal.pone.0208542.
Ugwu NH, Igwe I, Nwokeoma BN, Ajuzie HD, Iwuamadi KC, Ezike SC, Madukwe CI (2022).
Adolescents’ knowledge and use of sexual and reproductive health services in
the Federal Capital Territory, Nigeria. Afr J Reprod Health 26 (6): 80-88.
Unadike BC, Ekrikpo UE and Bassey EA (2012).
Awareness, Knowledge and perception of HIV/ AIDS and sexual behaviour amongst
Pre- Clinical, Medical Students in a Nigerian University. Nigerian Journal of
medicine. 21(3): 272- 276.
UNAIDS (2022). Global HIV and AIDS Statistics- Fact Sheet.
Available from: http://www.unaids.org.
Van der SluisW, Bouman M, de Boer N, Buncamper M,
van Bodegraven A, Neefjes-Borst
E (2016). Long-term follow-up of transgender women after secondary intestinal vaginoplasty. J Sex Med :13(04):702–710
Waktole ZD
(2019). Sexual behaviours and associated factors among youths in Nekemte town, East Wollega Oromia, Ethiopia. A cross sectional study. PLoS ONE
14(7): e0220235 http://doi.org/10.1371/journal.pone 0220235.
|
Cite this Article: Nwachukwu, C; Azuoma
KE; Ugwunze, AU; Enwelum,
HO; Nwozor, CM (2022). Assessment of Knowledge of
HIV and its Impact on the Sexual Behaviour of Chukwuemeka
Odumegwu Ojukwu
University (COOU) Students, Igbariam Campus. Greener Journal of Medical Sciences,
12(1): 178-184.
|




