By Enebili, V; Abhulimen, V; Eyimina, P (2023).
Fixation of Traumatic Femoral Shaft Fracture
in Port Harcourt: Comparison of Locked Intramedullary Nailing and Plating.
Enebili, Victor; Abhulimen, Victor; Eyimina,
Philip
Urology Division, surgery department,
University of Port Harcourt Teaching Hospital, Port Harcourt.
|
ARTICLE INFO
|
ABSTRACT
|
|
Article No.: 022823018
Type: Research
Full Text: PDF, HTML, PHP, EPUB
DOI: 10.5281/zenodo.7927503
|
Background: Trauma is increasingly becoming a public health concern worldwide.
Femoral fractures resulting from trauma are challenging to manage.
Definitive stabilization of the fractured
femur shaft could be done by various methods. Locked intramedullary nailing
is the gold standard for surgical stabilization and plating are two options
for management. Both methods have advantages and disadvantages.
Method: This is a prospective randomized study conducted in two centres,
located in Port Harcourt metropolis over a period of twelve months. Ethical
approval was obtained from both hospitals and informed consent was obtained.
Data were analysed using Statistical Package for Social Science (SPSS)
version 20. Results were presented in graphs and tables.
Result: A total of 70 patients completed the study with 35 in each group. Males
were more in number. The commonest cause of injury was motor vehicular
accidents with n= 16 (45.7%) in the nailing group and n= 24 (68.6%) in
plating group. The average time to weight bearing was 4 weeks for nailing and
9.26 weeks for plating. Also, the average time to return to normal activity
was 8.31 weeks for nailing and 14.09 weeks for plating. The average time to
early bony union was 14.49 weeks for nailing and 18.69 weeks for plating.
Conclusion: Fixation of traumatic femoral shaft fracture using locked
intramedullary nailing resulted in a shorter duration of hospital stay and
early commencement of normal duties.
|
|
Accepted: 01/03/2023
Published: 11/05/2023
|
|
*Corresponding
Author
Enebili, Victor
E-mail: victorabhulimen80@ gmail.com
|
|
Keywords: Trauma,
Femoral shaft fracture, Interlocking nailing, Plating.
|
|
|
|
INTRODUCTION
Trauma
is the bane of an industrialized society. The manufacture of fast-moving
vehicles and high-calibre weapons has increased its
incidence and is thus a growing public health burden worldwide1-4Femoral
shaft fracture is a common injury and usually follows high-energy trauma in
young men, mostly from road traffic crashes, gunshot injuries and falls from
heights3-7
Femoral shaft
fracture is often associated with injuries to other body systems and could be
complicated by severe haemodynamic instability, fat
embolism, acute respiratory distress syndrome, and multiple organ dysfunction4,5,6. Femoral shaft fractures are amongst the major
injuries following trauma that an orthopaedic surgeon
will commonly manage.5
Management of
traumatic femoral shaft fracture is divided into initial resuscitation, later
definitive stabilization of the fracture and treatment of other injuries
depending on their severity3,4,6. Various
methods of treatment of femoral shaft fracture include traction with or without
cast bracing, external fixation, plating and intramedullary nailing5,6,7. Conservative management of femoral shaft fracture
had been with traction and cast bracing8 but the high rate of
complications such as malunion and knee joint
stiffness together with problems of prolonged immobilization have made such
treatment unpopular. Conservative management is however an option of treatment
in resource-poor countries and occasionally when temporary stabilization is
required before definitive surgery2,9. The
use of an external fixator is generally reserved for open fractures and as a
damage control procedure for polytraumatized patients
not fit for a long duration of surgery3,6.
Fixation with locked
intramedullary nails (Locked nailing) is believed to be the gold standard for
most femoral shaft fractures6,7,8,910,11.
Its advantages include restoration of length, rotational stability and early
functional use of the extremity9,10,11. The
use of interlocking nails which acts as internal splinting also shows
superiority with a short hospital stay, low non-union rate and low infection
rate. This method of fixation however requires an image intensifier and
fracture table. The Surgical Implant Generation Network (SIGN) nailing system
was designed to be used in resource-poor areas where fracture table and
intraoperative imaging may not be available2,9,12,13,14.
The SIGN nail has allowed the use of locked intramedullary nails in many centres in Nigeria for humeral, femoral and tibial diaphyseal fractures.13,14
A retrospective study
on intramedullary nailing has been carried out by Furo
et al.15 but none comparing the outcome of
intramedullary nailing and plating in Port Harcourt. We
are unaware of any study conducted in Port Harcourt, Rivers state comparing
both methods of femoral fixation. The essence of this study is to
scientifically compare interlocking nailing and plating methods of fixation of
traumatic femoral shaft fracture in a resource-limited region.
MATERIALS AND METHODS
This study was
carried out on adults with fresh traumatic femoral shaft fractures who
presented for treatment within two weeks of injury in Port Harcourt metropolis.
This was a prospective randomized study involving the two tertiary care centres in Port Harcourt, Nigeria over a period of twelve
months. This study was conducted at the University of Port Harcourt Teaching
Hospital and Braithwaite Memorial Specialist Hospital both in Port Harcourt
metropolis. Patients were then followed up in the Orthopaedic
Outpatient Clinic of the respective hospitals after discharge.
The patients that
were included in the study were patients aged between 18 to 65 years with fracture
of the femoral shaft who presented to either the University of Port Harcourt
Teaching Hospital or Braithwaite Memorial Specialist Hospital both in Port
Harcourt for treatment within two weeks of injury during the study period.
Patients with medical co-morbidities unfit for surgical stabilization,
pathological fractures, non-union of the femoral shaft, More than Type 1 open
fracture of the femur using Gustilo et al
classification, below 18 years and above 65 years were excluded from the study.
Recruited patients were allotted into either nailing or plating group based on
random sampling by balloting. The research assistant wrote down alphabets A and
B in equal numbers for patients to choose from. Those who choose A were in the
nailing group, while those who choose B were in the plating group.
Patients, who met the
inclusion criteria and accepted to be recruited for the study, signed an
informed consent form. Then at the emergency unit, quick history was taken, and
then patients were adequately resuscitated using the Advanced Trauma Life
Support protocol when necessary. Detailed history and good clinical examination
were done on these patients after adequate resuscitation. Radiological
investigation of the fracture and other injuries if any was done to classify
and determine fracture pattern, Packed Cell Volume and Urinalysis was requested
and those with Packed Cell Volume of less than 27% were transfused as required.
Other investigations done are Electrolyte, Urea and Creatinine,
and chest radiographs for hypertensive patients and those above 40 years. Blood
sugar estimation to rule out diabetes was done.
Fractures were
classified using the AO/OTA classification system of femoral shaft fracture. An
adequate preoperative anaesthetic review was carried
out to determine fitness for surgery and anaesthesia.
Patients were on preoperative fasting for at least 6 hours. All information
obtained was adequately entered into the proforma/
questionnaire. The choice of anaesthesia was spinal anaesthesia except when contraindicated. Prophylactic
antibiotic Ceftriaxone 1 gram was given at the commencement of anaesthesia.
For plating, exposure
to fracture was done through a posterolateral
approach down to the fracture site. The fracture was reduced under direct
vision and the appropriate stainless steel broad dynamic compression plate
(DCP) was placed and then secured with cortical screws with at least eight
cortices above and below the fracture site.
For interlocking
nailing, SIGN instrumentation was used and the fracture site was opened through
a mini direct posterolateral approach down to the
bone. The fracture was then reduced under direct vision. The entry point for
the nail was either the greater trochanter for antegrade
nailing or the intercondylar ridge of the femur for
retrograde nailing depending on the location of the fracture on the shaft.
Reaming of the intramedullary canal was done to chatter then an appropriately
sized nail 2 sizes below the last reamer used to
obtain chatter was introduced into the medullary canal and then locked with
SIGN cortical locking screws.
A drain was placed
and the wound was dressed with sterile material after wound closure in both
plating and nailing.
Postoperatively,
patients were monitored for haemodynamic stability in
the recovery room. Adequate analgesia was given (Pentazocine
and Diclofenac suppositories. Ceftriaxone 1 gram
daily was continued for at least another 48 hours post-operatively. Patients
commenced oral feeds once they can communicate intelligently.
The drain was removed
on the 5th day postoperatively while sutures were removed on the 14th day
postoperatively and then discharged on the 14th postoperative day.
Patients were followed up in the outpatient clinic initially at 2 weeks after
discharge from the hospital then monthly for at least 6 months. Assessing for
clinical and radiological union was done at 6, 12 and 24 weeks. For this study,
clinical union was said to have been achieved when pain is absent at the site
and painless weight bearing. While radiological union is when there is the presence
of bridging callus or absence of fracture line on a plain radiograph.
Physiotherapy was commenced soon after surgical stabilization and was done in
the physiotherapy department of the hospital.
The sample size was
calculated using the formula52 for the comparison of two groups
|
n=
|
(u + v)2
|
(ó21 + ó20)
|
|
|
|
|
(µ1- µ0)2
|
Where
n= the minimum sample
size
µ1- µ0=
difference between the means
ó1
+ ó0= standard deviations
+u = the power required
at a 95% confidence interval, 1.64
v= significance level
required, 1.96
µ1= the meantime of full union of femoral shaft fracture
using the plating method was gotten from a study by Ogunlade
et al16 = 20.0 weeks
µ0= the mean of time of full union of femoral shaft fracture
using interlocking (SIGN) nail method, was gotten from a study by Ikpeme et al13 = 16.9 weeks
ó1 = the Standard deviation of time of full union of
femoral shaft fracture using the Plating method = 4.0 weeks
ó0 = the Standard deviation of time of full union of
femoral shaft fracture using Interlocking (SIGN) nail method = 5.4 weeks
|
n=
|
(1.64+1.96)2
|
(4.02+5.42)
|
|
|
|
|
(20–16.9)2
|
|
n=
|
(3.6)2
|
(16 + 29.16)
|
|
|
|
|
(3.1)2
|
n=60.90
The sample size for
both groups will be approximately 61 or all samples check.
Compensating for
non-response, assuming an attrition of 10% (response rate of 90%), the minimum sample size is
Ns= n/0.9
Ns= 61/0.9
= 67.8 for both groups.
Minimum sample size =
68 or all samples checked.
Data collected were analysed using the Statistical Package for Social Sciences
(SPSS) for windows version 20. Observed differences between the two groups were
tested for statistical significance using the Pearson Chi-square test for
association between categorical variables and the student t-test to compare the
association between means. The level of significance was set as p < 0.05.
The result was presented by descriptive statistics using tables of frequency
count, percentages and graph presentations while the research hypotheses were
tested using appropriate statistical techniques and as an inferential analysis
to test the relatedness of the research objectives and findings.
Consultants in both
hospitals supervised the research and performed the surgeries. Two senior
registrars and nurses in both hospitals assisted in the emergency room,
operating theatre and outpatient clinic. The study protocol was given to all
participants and their various roles were discussed in order to full
cooperation and involvement. A research assistant supervised the random
sampling.
Ethical approval was
obtained from the research and ethics committees of the University of
Port-Harcourt Teaching Hospital and Braithwaite Memorial Specialist Hospital in
line with the Helsinki declaration.
RESULTS
A total of eighty-two
(82) patients were recruited for the study during the periods. Seven (7)
patients were lost to follow-up at different periods during the study while
five (5) patients were excluded because of age, mechanisms of injury and
duration between injury and presentation to the hospital. A total of seventy
(70) patients however completed the study and were analyzed.
Socio-Demographic Characteristics of Patients in the
Study
The socio-demographic
characteristics examined include age distribution, sex distribution,
educational level and occupation in both the nailing and plating group. The age
most prevalently affected was between 30 - 40 years with 16 patients (45.7%) in
the nailing group and 10 patients (28.6%) in the plating group. The sex distribution
shows a male preponderance with 20 patients (74.3%) in the nailing group and 25
patients (71.4%) in the plating group while females accounted for a lesser
number with nine patients (25.7%) in the nailing group and 10 patients (28.6%)
in the plating group. The most frequently occurring educational level was the
tertiary level of education with 25 patients (71.4%) in the nailing group and
22 patients (62.9%) in the plating group. The most frequent occupation of the
patients among the study population was civil servants with
11 patients (31.4%) in the nailing group and nine patients (25.7%) in the
plating group distribution of the demographics is as shown in table 1.
The differences in proportions of the sociodemographic
variables were not statistically significant (p<0.05).
Table 1: Comparison of the socio-demographic
characteristics of patients between groups in the study
|
|
Groups in the study
|
|
|
Socio-demographic characteristics
|
Nailing
N=35
n (%)
|
Plating
N=35
n (%)
|
Total
N=70
n (%)
|
|
Age distribution
|
|
|
|
|
≤ 20 years
|
1 (2.9)
|
2 (5.7)
|
3 (4.3)
|
|
21 – 30 years
|
10 (28.6)
|
10 (28.6)
|
20 (28.6)
|
|
31 – 40 years
|
16 (45.7)
|
10 (28.6)
|
26 (37.1)
|
|
41 – 50 years
|
5 (14.3)
|
8 (22.9)
|
13 (18.6)
|
|
51 – 60 years
|
3 (8.6)
|
4 (11.4)
|
7 (10.0)
|
|
> 60 years
|
0 (0.0)
|
1 (2.9)
|
1 (1.4)
|
|
|
Fisher’s exact test=3.608; p-value=0.657
|
|
|
Sex distribution
|
|
|
|
|
Female
|
9 (25.7)
|
10 (28.6)
|
19 (27.1)
|
|
Male
|
26 (74.3)
|
25 (71.4)
|
51 (72.9)
|
|
|
Chi Square=0.072; p-value=0.788
|
|
|
Educational level
|
|
|
|
|
Primary
|
1 (2.9)
|
0 (0.0)
|
1 (1.4)
|
|
Secondary
|
9 (25.7)
|
13 (37.1)
|
22 (31.4)
|
|
Tertiary
|
25 (71.4)
|
22 (62.9)
|
47 (67.1)
|
|
|
Fisher’s exact test=1.847; p-value=0.440
|
|
|
Occupation
|
|
|
|
|
Student
|
10 (28.7)
|
8 (22.9)
|
18 (25.7)
|
|
Trader/Business
|
6 (17.2)
|
10 (28.7)
|
16 (22.8)
|
|
Professional
|
3 (8.6)
|
3 (8.6)
|
6 (8.5)
|
|
Civil servant
|
11 (31.4)
|
9 (25.7)
|
20 (28.5)
|
|
Skilled worker
|
5 (14.3)
|
5 (14.3)
|
10 (14.2)
|
|
|
Chi square=9.90 p-value=0.769
|
|
Cause of Injury
The major cause of
injury was motor vehicle injuries with 16 (45.7%) in the nailing group and 24
(68.6%) in the plating group, followed by Motor cycle injuries which accounted
for seven (20.0%) in the nailing group and five (14.3%) in the plating group. The
distribution of other causes of injury in the two groups is shown in figure 1.
The differences in the proportion of the causes of injury between the two
groups were not statistically significant (p >0.05).

Figure 1: Distribution of causes of injury across study
groups
Location of Fracture on the Shaft
The proximal part of
the femoral shaft was the location of the fracture among three (8.6%) patients
in the nailing group and four (11.5%) patients in the plating group. The middle
part of the femoral shaft was noticed to be the location of the fracture (77.1%)
patients in the nailing group and 25 (71.4%) patients in the plating group
while the distal part of the femoral shaft was the location in five (14.2%)
patients in the nailing group and six (17.1%) patients in the plating group.
The differences in the proportion of the location of the fractures on the shaft
between the two groups were not statistically significant (p >0.05).

Figure 2: Distribution of location of injury across study
groups
Laterality of Fracture
The left limb
accounted for fracture in 17 (48.6%) patients of the nailing group and in 18
(51.4%) patients of the plating group. Also, among the nailing group fracture
was located on the right limb in 12 (34.3%) patients while for the plating group,
the right limb was the location in 23 (65.7%) patients.

Figure 3: Laterality of fracture across study groups
AO CLASSIFICATION OF THE FRACTURES
A comparison of the f
AO Classification of the fractures showed that B2 fractures were the most
common fracture type in both groups accounting for 11(31.4%) in the nailing
group and 11 (31.4%) in the plating group. The distribution of other fracture
types is shown in table 2. The differences in proportions were not
statistically significant (p >0.05).
Table 2: Comparison of AO Classification of the fractures
between groups
|
|
Groups in the study
|
|
|
AO Fracture type
|
Nailing
n (%)
|
Plating
n (%)
|
Total
n (%)
|
|
A1
|
1 (2.9)
|
2 (5.7)
|
3 (4.3)
|
|
A2
|
8 (22.9)
|
6 (17.1)
|
14 (20.0)
|
|
A3
|
9 (25.7)
|
11 (31.4)
|
20 (28.6)
|
|
B1
|
4 (11.4)
|
2 (5.7)
|
6 (8.6)
|
|
B2
|
11 (31.4)
|
11 (31.4)
|
22 (31.4)
|
|
B3
|
1 (2.9)
|
3 (8.6)
|
4 (5.7)
|
|
C2
|
1 (2.9)
|
0 (0.0)
|
1 (1.4)
|
|
Total
|
35 (100.0)
|
35 (100.0)
|
70 (100.0)
|
|
|
|
|
|
Fisher’s exact test=3.473; p-value = 0.804
Duration of Hospital Stay between Groups in the Study
There was no
significant difference noticed in the mean duration of hospital stay between
the nailing and the plating group across the different causes of injury
(p>0.05).
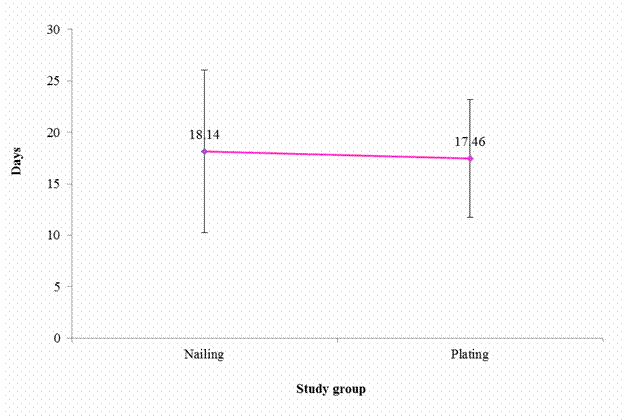
Figure 4: Comparison of the average time between surgery
and discharge between groups in the study
Time to Weight Bearing Between Groups in the Study
The mean time to
weight bearing was significantly lower among the nailing group in comparison to
the plating group (p<0.05). There was no case of assault among the nailing
group. There was also no case of auto-pedestrian injury among the plating
group.

Figure 5: Comparison of the average time to weight
bearing between groups in the study
Time to Return to Normal Activity between Groups in the
Study
The mean time to
return to normal activity was significantly lower among the nailing group in
comparison to the plating group (p<0.05).

Figure 6: Comparison of the average time to return to
normal activity between groups in the study
Time Interval between Surgery and Return to Work
The mean time
interval from surgery to return to work was significantly lower among the
nailing group in comparison to the plating group in those whose cause of injury
was RTC motor vehicle (10.75±3.91 vs. 16.33±3.0), and overall (10.60±3.69 vs.
15.71±3.42) p<0.05. There was no case of assault among the nailing group.
There was also no case of auto-pedestrian injury among the plating group and
there was no significant difference noticed between the mean time from surgery
to work among the nailing group in comparison to the plating group among those
who fell from height and those with RTC by motorcycle (p<0.05).

Figure 7: Comparison of the mean time interval from
surgery to return to work between groups in the study
Time to Bony Union between Groups in the Study
The mean time to bony
union was significantly lower among the nailing group in comparison to the
plating group in those whose cause of injury were fall from height, gunshot,
RTC motor vehicle, RTC motorcycle and overall (p<0.05). There was no case of
assault among the nailing group. There was also no case of auto-pedestrian
injury among the plating group.

Figure 8: Comparison of the meantime to bony union
between groups in the study
Distribution of Complications
Among the nailing
group range of knee motion <110 and rotational deformity were the most
common complication three (8.5%) seen while haemorrhage
and infection were the least common complication noticed (2.9%). Among the
plating group haemorrhage, was the commonest
complication seen in five (14.3%) while rotational deformity and limb length
discrepancy were the commonly noticed
one (2.9%).

Figure 9: Distribution of complications across study
groups
Blood Transfusion
One (2.9%) patient
was transfused in the nailing group compared to four (11.4%) patients in the
plating group.

Figure 10: Distribution of blood transfusion across study
groups
Direct Cost of Hospital Bill
The estimated average
direct financial cost of nailing and plating for a mean total number of
hospital stay of 28 days for nailing and 32 days for plating. The direct
financial cost for nailing was two hundred and nineteen thousand naira compared
to two hundred and ten thousand naira.
Table 3: Average cost of hospital bill between study
groups
|
Charges
|
Rate (N)
|
Nailing group (N)
|
Plating group (N)
|
|
Implant
|
-
|
50,000
|
35,000
|
|
Surgery fee
|
-
|
90,000
|
90,000
|
|
Nursing care
|
500/ day
|
14,000
|
16,000
|
|
Bed fee
|
1000/ day
|
28,000
|
32,000
|
|
Radiograph
|
1500/ view
|
12,000
|
12,000
|
|
Physiotherapy
|
-
|
10,000
|
10,000
|
|
Pharmacy
|
-
|
15,000
|
15,000
|
|
TOTAL
|
|
219,000
|
210,000
|
DISCUSSION
Traumatic fracture of
the femoral shaft is common in our environment and is a major cause of
morbidity and mortality in the young population. Surgical fixation of femur
shaft fracture aims to maintain alignment, restore length, achieve bony union
and return the patient to pre-injury function as early as possible. However,
this has to be at an affordable cost to both the patient and the hospital.
The age group most
affected in this study is the 31- 40 year age group in both the nailing and
plating groups which was closely followed by the age group 21-30 years. This is
in keeping with various studies where persons below 40 years are mostly
affected. Kortor et el17
in Lagos reported a mean of 43.1 years, and Naeem-Ur-Razaq et al18 reported a mean of 37.05 years in
Abbottabad. Understandably, people younger than 40 years are the active
workforce in most societies and are involved in daily economic and recreational
activities in the community which puts them at risk of traumatic events. In
this study persons younger than 40 years contributed 77.2% (n=35) for the nailing
group and 62.9% (n=35) for the plating group while persons older than 60 years
was just one 2.9% (n=35) in the plating group and none in the nailing group. There
was a male preponderance in this study with males contributing 72.9% (n=70) of
traumatic femoral shaft fractures as against 27.1% (n=70) of females. This
pattern was similar to that of Kortor et el.17 reporting a ratio of 2.2:1. Males are breadwinners
of most families and are responsible for their financial demands. However, with
increasing advocacy for female education and empowerment this trend may be
reversed in the future. The highest proportion of professional groups in this
study were civil servants accounting for 31.4% (n=35) of nailing and 25.7%
(n=35) of plating while others are professionals and businessmen. These
patients have dependents and with the current national minimum wage set at thirty
thousand naira,19 the economic impact of fixation by either method
cannot be overemphasized hence a fixation method that returns patients to work
early and is also cost-effective will be most preferred.
The commonest
mechanism of injury in both groups was motor vehicle crashes which accounted
for 45.7% (n=35) for the nailing group and 68.6% (n=35) for the plating groups
respectively. This is closely followed by motorcycle crashes at 20.0% (n=35)
for the nailing group and 14.3% (n=35) for the plating group. The reduction in
motorcycle crashes may result from the ban on motorcycles for commercial
purposes in Port Harcourt, Rivers state. Older North American studies show similar
reports.20,21 More recent North American studies reveal osteoporosis
from ageing as a common cause.22,23 Additionally, the energy
transfer in motor vehicle crashes is far higher than in motorcycle crashes
because of their velocity at the time of impact. In this study, gunshot injury
only contributed 5.7% (n=35) each for both the nailing and the plating group.
The few cases may be due to reduced presentation to hospitals to avoid police
interrogation and arrest24 since the majority of gunshot wounds
result from civil unrest and criminality.3,4
Also, most fractures resulting from gunshot injuries are often high-grade open
fractures and would have been excluded from this study.
The mean duration to
weight bearing was shorter in the nailing group, with an average of 4.00 weeks
for nailing compared to 9.26 weeks for the statistically significant plating
group. This may be because the nail is a load-sharing implant with a widespread
bone interface compared to a plate that is a load-bearing implant. Thus, after
nailing patients can bear weight earlier without the risk of implant breakage
compared to the plating. The mean duration to commence normal activity was
significantly shorter in the nailing despite the cause of injury, with an
average of 8.31 weeks for nailing and 14.09 weeks for plating which was
statistically significant. The interlocking nail is a load-sharing implant and
provides axial and rotational stability with no stress riser effect of multiple
screws holes in the shaft of the femur, thus it can sustain high stress of
ambulation without failure compared to compression plating which is a load-bearing
implant with multiple screw holes and stress riser effect.
The duration of bony
union was shorter in the nailing group compared to the plating group, with an
average of 14.49 weeks for nailing and 18.69 weeks for plating which was
statistically significant. This may be because the nail provides relative
stability and such fixation has the tendency to heal by secondary bone healing
producing florid callus initially that are readily visualized on x-ray compared
to a plate that is used to achieve absolute stability resulting in direct bone
healing with minimal callus around the fracture site. However, both nailing and
plating have been reported to have high bone union rate12-14
Analysis of postoperative
complications showed that haemorrhage (greater than
1.5L blood loss) and infection (superficial surgical site infection) were the
major complications in the plating group while rotational deformity and limb
length discrepancy (greater than 2cm) were the major postoperative
complications in the nailing group. In total there were more complications seen
in the plating group than in the nailing group. Complications were seen in 15
patients in the plating group and 10 patients in the nailing group.
Significant haemorrhage requiring transfusion was seen in 5 patients in
the plating group and only 1 patient in the nailing group. While
infection was seen in 4 patients in the plating but only 1 patient in the
nailing group had a superficial surgical site infection. This can be
attributed to the larger soft tissue exposure, wider periosteal stripping and
longer duration of surgery in the plating group. Chaudhary
et al.25 reported a higher incidence of blood loss from plating than
nailing humeral shaft fracture and Bostman et al.26
reported a higher incidence of both deep and superficial infection from plating
than nailing femoral shaft fractures. The average duration of surgery in the
plating group was 2 hours and 15 minutes while it was 1 hour and 30 minutes in
the nailing group. However, the surgeon’s technique, experience and theatre
design are other contributory factors, hence this may not be universal.
Rotational deformity
was seen in 3 patients in the nailing group and 1 patient in the plating group.
Limb length discrepancy was seen in 2 patients in the nailing group and 1
patient in the plating group. While plating aims to achieve anatomic reduction
and rigid fixation, nailing which aims to achieve functional reduction and
relative stability. This may account for the significantly higher proportion of
rotational deformity in the nailing group.
The cost of the implant
showed that the nail implant is more expensive than the plate with fifteen
thousand naira and the total estimated hospital bill is also higher in patients
who had nailing compared to those who had plating with a difference of nine
thousand naira. Although the plating group spent a longer duration in the hospital
with an average of 32 days compared to the nailing group which spent an average
of 28 days in the hospital. This difference in the estimated cost of hospital bills
is marginal as patients who can afford plating could also afford the yearly
cost of care for nails. The long duration of the hospital stay was due to a delay
in surgical fixation and physiotherapy mobilization.
CONCLUSION
Operative fixation is
an excellent method of fixation of traumatic femoral shaft fractures. Open
interlocking nailing and plating of traumatic femoral shaft fractures both have post-operative complications. While haemorrhage
and infection are common with the plating of these fractures, rotational
deformity and limb length discrepancy are common with nailing. Open
interlocking has the advantage of early return to normal occupational activity
for traumatic femoral shaft fracture. Both techniques have a high bony union
rate for traumatic femoral shaft fracture with the interlocking nailing
providing a better early outcome compared to the plating.
RECOMMENDATION
Open intramedullary
nailing and plating are ideal options for treatment for traumatic femoral shaft
fracture as they have reduced hospital stay, early return to work and high
union rate. All adults should be offered these methods of treatment of femur
shaft fracture, open intramedullary nailing
additionally has a lower rate of infection and haemorrhage
than plating and should be considered as a first-line treatment option for
traumatic femoral shaft fracture.
LIMITATIONS
The
duration of the study was limited by a short follow-up period due to the
expected time to submit the dissertation to the postgraduate college for
assessment. The study was interrupted by several industrial actions and several
upward reviews of the cost of implants and surgery.
SOURCE OF FUNDING
The
research was funded by the authors.
ACKNOWLEDGEMENTS
We
acknowledge our colleagues who supported us throughout the period of this
research. We also thank our spouses, without them this work will not have been
completed.
REFERENCES
1.
Aduful HKA, Adu-Aryee
NA, Anyanwu CH, Archampong
EQ, Yeboah ED, Dakorah TK,
Management of the injured patient: Penetrating and non-penetrating injuries. In
Badoe EA, Archampong EQ, da
Rocha-Afodu JT, eds. Principles and practice of
Surgery including pathology in the tropics 4th Edition. Accra:
Assemblies of God Literature Centre Ltd, 2009; 159-198.
2.
Sekimpi P, Okike K,
Zirkle L, Jawa A. Femoral
fracture fixation in developing countries: an evaluation of the Surgical
Implant Generation Network (SIGN) intramedullary nail. J Bone Joint Surg Am 2011; 93: 1811 – 1818.
3.
Obene TA, Abhulimen
V. Presentations of gunshot injuries to the extremities in a tertiary hospital
in Port Harcourt. International Surgery Journal. 2022 Sep 28;9(10):1689-93.
4.
Obene TA, Abhulimen
V, Richard E. Evaluation of Gunshot Wounds to the Extremities: Correlation of
Red Cross Wound Score and Initial Response to Management. American Journal of
Health, Medicine and Nursing Practice. 2022 Sep 14;7(11):9-21.
5.
Whittle
AP. Fracture of the lower extremity. In Canale ST, Beaty TH, eds. Campbell’s operative orthopaedics
11th Edition, Philadelphia; Mosby Elsevier, 2008; 3085-3236.
6.
Nayagam S. Injuries of the hip and femur. In
Solomon L, Nayagam S, Warwick D, eds. Apley’s system of orthopaedics
and fractures, 9th Edition London: Hodder
Arnold, 2010; 843-873.
7.
Nork SE. Femoral Shaft fracture. In Bucolz RW, Court-Brown CM, Heekman
JD, Tornetta P eds. Rockwood and Green’s Fracture in
adults. 7th edition by. Lippincott Williams and Wilkin 2010.
8.
Koval KJ, Zuckerman PD, Chapt
32. In Handbook of fractures, 3rd Edition. Lippincott Williams and
Wilkins 2006.
9.
Charnley J. conservative versus operative
methods. In Charnley J ed.
The closed treatment of common fractures 3rd edition. Edinburgh:
Churchill Livingstone 1961; 1-42.
10.
Winquist RA. Locked femoral nailing: J Am Acad Orthop Surg
1993; 1: 95-105.
11.
Bong
MR, Kummer FJ, Koval KJ, Egol KA. Intramedullary Nailing of the lower extremity:
biomechanics and biology. J Am Acad Orthop Surg 2007; 15: 97 – 106.
12.
Chakraborty MK, Thapa P, Sathian B. Surgical
Implant Generation Network (SIGN) solid intramedullary interlocking nail in the
lower extremity: an observational study from western Nepal. J Clin Diagn Res 2011; 5: 1614 –
1617.
13.
Ikpeme I, Ngim N, Udosen A, Onuba O, Enembe O, Bello S, External jig aided intramedullary nail
of diaphyseal fracture: an experience from a tropical
developing centre. IntOrthop2011; 35: 107 -111.
14.
Ikem IC, Ogunlusi
JD, Ine HR, Achieving interlocking nails without the use
of image Intensifier. Int Orthop
2007; 31: 487 -490.
15.
Orupabo F, Harcourt S, Eyimina
PD. Interlocking nailing of lower limb fractures at the University of Port
Harcourt Teaching Hospital. The Nigerian Health Journal. 2021;21(3):114-22.
16.
Ogunlade SO, Alonge
T, Omololu B, Ifesanya A, Nottidge T, Diete-Spiff T.
Plating of femoral shaft fractures: The experience in an African Teaching
Hospital. Eur J Trauma Emerg
Surg 2007; 33:613 – 618.
17.
Kortor JN, Yinusa
N, Ugbeye ME. Lower limb injuries arising from
motorcycle crashes. Niger J Med 2010,
19: 475 -478.
18.
Naeem-Ur-Razaq M,
Qasim M, Khan MA, Sahibzada
AS, Sultan S. Management outcome of closed femoral shaft fractures by open
Surgical Implant Generation Network (SIGN) interlocking nails. J Ayub Med Coll Abbottabad. 2009;
21: 21 -24.
19.
Musti BM, Mallum
A. An assessment of the effect of casual employment on the level of poverty and
economic growth in Nigeria. JBED. 2020;5 (3):172-7.
20.
Winquist RA, Hansen ST, Clawson DK. Close
Intramedullary nailing of femoral fracture. a report
of five hundred and twenty cases. J Bone Joint Surg
Am 1984; 66: 529 -539.
21.
Bone
LB, Johnson KD, Weigelt J, Scheinberg
R. Early versus delayed stabilization of femoral fractures. a
prospective randomized study. J Bone Joint Surg Am
1989; 71: 336 -340.
22.
Shelton
C, White S. Anaesthesia for hip fracture repair. BJA
education. 2020 May;20(5):142.
23.
Fischer
H, Maleitzke T, Eder C, Ahmad S, Stöckle
U, Braun KF. Management of proximal femur fractures in the elderly: current
concepts and treatment options. European Journal of Medical Research. 2021 Dec;26:1-5.
24.
Odatuwa-Omagbemi DO,
Adiki TO. Pattern at the presentation of extremity
gunshot injuries in Warri, Nigeria. The Nigerian Health Journal 2013; 13: 85 –
90.
25.
Chaudhary P, Karn NK, Shrestha BP, Khanal GP, Rijal R, Maharjan R, Kalawar RP,
Randomized control trial comparing dynamic compression plate versus
intramedullary interlocking nail for management of humeral shaft fracture.
Health Renaissance 2011; 9: 61 – 66.
26.
Bostman O, Varjonen
L, Vainionpaas S, Majola A,
Rokkanen P. Incidence of local complications after
intramedullary nailing and plate fixation of femoral shaft fractures. J Trauma
1989, 29; 5: 639 - 645.
|
Cite this Article: Enebili, V; Abhulimen, V; Eyimina,
P (2023). Fixation of Traumatic Femoral Shaft Fracture in Port Harcourt:
Comparison of Locked Intramedullary Nailing and Plating. Greener Journal of Medical Sciences, 13(1): 17-31. https://doi.org/10.5281/zenodo.7927503.
|










